
April 13, 2026
Learn how to tailor active rehab for professionals by balancing your schedule, maximizing therapy participation, and leveraging peer support for success.
Start Your Journey NowWritten and reviewed by the clinical team at Trifecta Healthcare Institute, a men’s-only treatment center in Tennessee specializing in substance use, mental health, and dual diagnosis care.
When seeking active rehab for professionals, understanding the biological impact of exercise is the first step toward lasting change. Physical activity directly influences the brain’s neurochemistry. When a person engages in structured exercise—such as the boxing, jiu-jitsu, or hiking programs offered at Trifecta Healthcare Institute—the body releases endorphins, dopamine, and serotonin. These neurotransmitters are responsible for mood regulation and reward processing.

They play a crucial role in supporting motivation, stress tolerance, and emotional stability, all of which are essential for sustained recovery4. Consider this method if you find traditional talk therapy alone leaves you feeling restless or disconnected from your physical body.
Research highlights that regular movement not only reduces symptoms of depression and anxiety, but also enhances cognitive flexibility. This is the ability to adapt to new challenges and routines, a skill especially valuable for professionals balancing recovery with demanding careers4. Furthermore, physical activity heightens neuroplasticity—simply put, the brain’s capacity to rewire itself and form new connections in response to experience.
"Movement-based recovery models can accelerate positive behavioral changes and support long-term abstinence by creating new, healthier habits and coping strategies that replace previous substance use patterns." — American Psychological Association4
This approach is ideal for professionals who require both mental acuity and emotional resilience in high-stakes environments. By integrating biohacking techniques like ice baths to restore neurochemical balance, men can actively participate in their healing. Next, it’s important to examine how these neuroscientific principles translate into day-to-day integration models for working professionals.
Active rehab for professionals focuses on blending therapeutic movement, peer support, and evidence-based modalities into day-to-day routines without disrupting career momentum. Integration models range from early-morning group sessions before office hours, to lunchtime fitness-based therapy, to evening peer meetings—each tailored to the realities of a professional’s week.
This strategy suits professionals who need recovery support that complements, rather than conflicts with, work obligations. For instance, if you're a small business owner with rigid operating hours, evening intensive outpatient programs (IOP) might be necessary. Conversely, an enterprise executive with heavy travel might pair intensive group exercise blocks with remote check-ins, allowing for continued participation during business trips8.
The rise of flexible outpatient and telehealth-driven programs is projected to accelerate sector growth, driven by professionals’ demand for convenience, privacy, and personalized care8. Programs that explicitly address confidentiality—such as those with private entrances or secure digital platforms—help maintain trust and engagement among career-focused participants5. Adopting integration models that align with professional responsibilities ensures sustained recovery without sacrificing upward mobility.
Before committing to a structured outpatient program, professionals need to conduct an honest evaluation of their current situation and readiness for change. This self-assessment forms the foundation of successful recovery and helps determine whether the timing aligns with both clinical needs and professional obligations. Whether you are looking for a Nashville rehab or a Knoxville rehab for men, understanding your baseline is critical.

The first consideration involves evaluating the severity and impact of substance use on daily functioning. Professionals should examine whether their use has created consequences in work performance, relationships, or physical health. Signs that this level of treatment may be appropriate include struggling to maintain productivity, experiencing withdrawal symptoms during work hours, or finding that substance use has become necessary to manage stress or anxiety.
| Readiness Factor | Standard Outpatient Profile | Intensive Outpatient (IOP) Profile |
|---|---|---|
| Time Commitment | Can dedicate 6-8 hours weekly | Can dedicate 9-15 hours weekly |
| Clinical Need | Mild to moderate support needed | Requires rapid stabilization and daily accountability |
| Co-occurring Symptoms | Managed stress or mild anxiety | Active trauma, depression, or severe anxiety |
Equally important is assessing practical readiness. These programs typically require a significant weekly commitment, often scheduled during evening hours to accommodate work schedules. Professionals must evaluate whether they can realistically dedicate this time while maintaining their career responsibilities. This includes considering upcoming project deadlines, travel commitments, and whether disclosure to employers or colleagues becomes necessary.
The presence of a support system also plays a critical role in recovery readiness. Professionals should consider whether they have trusted individuals who can provide accountability and encouragement throughout the process. For those who value privacy, men's-only programs operate on a brotherhood philosophy, offering a unique environment where peer support develops naturally among individuals facing similar challenges.
Mental and emotional readiness represents perhaps the most crucial factor. Recovery requires willingness to examine underlying patterns, confront uncomfortable truths, and commit to meaningful change. It is important to note that facilities like Trifecta Healthcare Institute provide co-occurring mental health treatment alongside substance use disorder support, rather than primary mental healthcare. This ensures that interconnected issues like trauma or anxiety are addressed holistically.
Physical readiness matters too, particularly for programs incorporating movement-based recovery approaches. Professionals should consider whether activities like boxing, hiking, or other physical therapies align with their interests and capabilities, as engagement with these modalities often enhances overall treatment outcomes and provides healthy coping mechanisms that extend beyond the clinical setting.
Active rehab for professionals often hinges on selecting a treatment structure that aligns with professional responsibilities and recovery goals. Outpatient programs suit those managing stable work schedules or seeking a gradual entry into structured recovery. This solution fits men who want to integrate therapy and movement without significant disruption to their careers, typically requiring an investment of $3,000 to $7,000 depending on duration and insurance coverage.
Intensive outpatient models cater to individuals experiencing higher stress, more severe symptoms, or who need daily accountability. Opt for this framework when rapid stabilization, greater peer support, or comprehensive co-occurring mental health care is essential. According to the American Psychological Association, IOPs can achieve outcomes comparable to full-time inpatient care for many working men, especially when paired with movement-based modalities4.
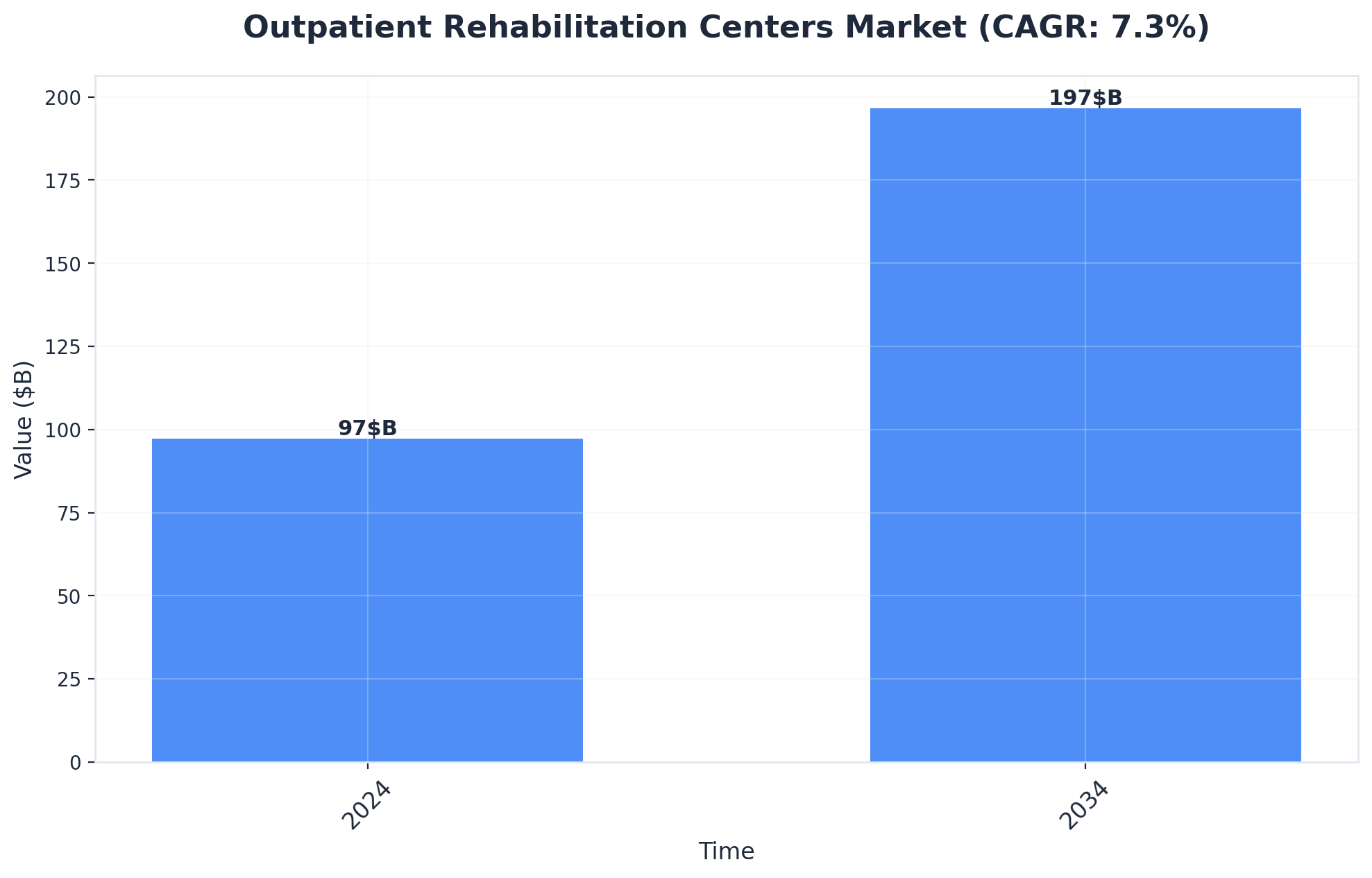
As demand for flexible, personalized treatment rises, outpatient rehabilitation centers are projected to double in market size by 2034, reflecting professionals’ desire for programs that adapt to their unique schedules8. Next, we’ll explore practical strategies for scheduling around career demands while sustaining progress in recovery.
Balancing career obligations with structured recovery can be challenging, but active rehab for professionals thrives on adaptable scheduling. Many programs now offer early morning or late evening sessions, allowing high-performing individuals to participate without sacrificing client commitments or leadership responsibilities.
To protect your privacy while blocking out time, use your calendar's privacy settings. For example, in most corporate email clients, you can press Ctrl + E to edit a calendar event, and set the visibility to Private. You can also use simple automation to ensure your recovery time is protected:
// Example Calendar Automation Concept function scheduleRecoveryBlock() { let event = CalendarApp.createEvent('Personal Development', startTime, endTime); event.setVisibility(CalendarApp.Visibility.PRIVATE); event.setGuestsCanSeeGuests(false); } This approach works best when professionals benefit from clear boundaries—such as setting calendar holds for therapy and group movement—while maintaining flexibility for urgent business needs. Strong coordination between clinical staff and participants ensures that rescheduling due to last-minute work changes does not disrupt progress, addressing a core concern for executives and consultants.
According to business research, demand for programs that blend in-person and virtual options continues to rise, particularly among men who must remain present in their industries while focusing on recovery8. The next section will guide you in translating these strategies into a concrete 30-90 day recovery plan that reinforces both professional and personal growth.
Creating a structured recovery plan bridges the gap between completing a comprehensive treatment program and sustaining long-term sobriety. The first 30 to 90 days post-treatment represent a critical transition period where relapse risk remains elevated, making intentional planning essential for professionals balancing recovery with career demands.
The initial 30 days should focus on solidifying daily routines that support neurochemical healing. This includes maintaining consistent sleep schedules, continuing evidence-based practices introduced during treatment, and establishing non-negotiable recovery activities. For professionals, this might mean scheduling morning workouts before work commitments or blocking calendar time for peer support meetings. The goal isn't perfection—it's building sustainable patterns that reinforce the neural pathways developed during structured treatment phases.
Physical activity remains crucial during this transition. Movement-based recovery programming helps restore dopamine and serotonin levels naturally, providing the neurochemical support that reduces cravings and improves mood regulation. Whether continuing boxing sessions, maintaining a hiking routine, or incorporating cold exposure practices, these activities serve dual purposes: they occupy time previously spent using substances and accelerate the brain's natural healing processes.
Days 31 through 60 should emphasize expanding your support network and testing boundaries. This phase involves gradually reintegrating into professional and social environments while maintaining recovery safeguards. Identify which networking events, client dinners, or professional obligations require modified approaches. Develop specific strategies for navigating situations where substances may be present, including exit plans and accountability check-ins with trusted peers from your recovery community.
The 60 to 90-day window focuses on refining what works and adjusting what doesn't. This period allows for honest assessment of which recovery tools provide the most value for your specific circumstances. Some professionals find that morning group therapy sessions fit better than evening options, while others discover that outdoor adventure activities provide more therapeutic benefit than traditional talk therapy alone. Use this time to customize your ongoing recovery approach based on real-world experience rather than theoretical planning.
Throughout all three phases, maintaining connection with your recovery community prevents isolation—a primary relapse trigger. Whether through alumni programming, peer support networks, or continuing care services, consistent engagement with others who understand the recovery journey provides accountability and perspective. This path makes sense for men in recovery, as these brotherhood connections often become the foundation for sustained sobriety, offering both practical support during challenging moments and celebration during milestones.
Recovery from substance use disorder requires more than good intentions—it demands structure, accountability, and a clear roadmap forward. The 30-90 day period following intensive treatment represents a critical window where new habits solidify and long-term patterns take shape. Professionals navigating this transition need programs that respect their existing commitments while providing meaningful support.
Structured outpatient treatment offers the flexibility to maintain career responsibilities while building sustainable recovery practices. By integrating evidence-based therapies with movement-based activities and peer support, men can develop the physical and emotional resilience necessary for lasting change. The key lies in creating systems that address both immediate challenges and long-term wellness.
Whether seeking Nashville drug rehab or Knoxville alcohol rehab, the right program should align with professional demands while fostering genuine transformation. Recovery isn't about perfection—it's about progress, consistency, and surrounding yourself with others committed to the same journey. With proper planning and the brotherhood support found at facilities like Trifecta Healthcare Institute, the path forward becomes not just manageable, but genuinely sustainable.
Outpatient programs in Tennessee for active rehab for professionals generally reflect the national trend toward cost-effective, flexible care. While exact pricing varies by provider, most outpatient rehabilitation centers are designed to be more affordable than inpatient or residential alternatives, partly due to fewer overnight and facility-related expenses. The outpatient segment's growth is fueled by professionals' demand for convenience and telehealth options—factors that can influence investment range and insurance coverage 8. Professionals can anticipate variable costs depending on session frequency, duration, and added services such as movement-based therapy, but should expect overall investments to align with the national outpatient market trajectory 8.
Men-specific programs create settings where participants engage with peers who share similar lived experiences, responsibilities, and communication styles. Unlike co-ed approaches, which may require additional focus on mixed-gender group dynamics, men’s programs often emphasize brotherhood, direct peer accountability, and activities tailored to male interests—such as boxing, martial arts, and competitive movement 4. This environment can reduce stigma, foster openness, and build trust more quickly, particularly for professionals who value privacy and peer-driven motivation in their recovery process. Active rehab for professionals in men-only groups may accelerate engagement and support emotional safety for those navigating high-stress roles 4.
Telehealth plays a crucial role in maintaining treatment continuity for professionals who travel frequently. Virtual therapy sessions, digital check-ins, and asynchronous support allow participants to remain engaged with movement-based programming and peer accountability regardless of location. This method works when unpredictable schedules or business travel would otherwise interrupt progress in active rehab for professionals. The Harvard Business Review notes that demand for hybrid and telehealth-enabled programs continues to increase among executives and consultants, as these solutions enable uninterrupted participation and confidential care—even from hotel rooms or remote offices 8. Consistent digital access helps bridge gaps, ensuring that recovery momentum is not lost during demanding travel periods.
Quality movement-based treatment providers are distinguished by credentials that go well beyond standard addiction counseling certifications. Look for clinicians licensed in addiction medicine or behavioral health, plus additional training in evidence-based physical activity modalities—such as physical therapy, exercise physiology, or trauma-informed movement practices. Programs recognized by professional associations like the American Psychological Association (APA) or the American Society of Addiction Medicine (ASAM) underscore clinical rigor and adherence to ethical standards 43. For active rehab for professionals, it’s also important that staff have experience integrating group exercise, peer support, and co-occurring mental health care for working adults. Transparency about clinician credentials and ongoing professional development signals a commitment to high-quality, results-driven care.
Co-occurring mental health support is integrated with substance use treatment through an approach known as dual diagnosis care. This means that professionals receive targeted support for both substance use and mental health challenges—such as anxiety, depression, or trauma—within the same treatment plan. Clinical teams coordinate evidence-based therapies (like cognitive behavioral therapy and movement-based modalities) to address the interplay between mood, stress, and substance use patterns. This method works best when providers screen for both mental health and addiction needs and adapt interventions in real time, ensuring comprehensive progress for those in active rehab for professionals 4.
Tennessee treatment programs for professionals prioritize confidentiality through federal regulations like HIPAA and 42 CFR Part 2, which strictly limit the sharing of personal health information without explicit consent. Many centers offer discreet intake procedures, private entrances, and secure digital platforms to protect participant identity—an approach that helps maintain trust for those in high-visibility roles 5. This path makes sense for professionals seeking active rehab for professionals who require assurance that details of their participation and clinical records remain confidential, protecting both reputation and career trajectory. Always verify that the provider’s privacy practices align with state and federal standards before enrolling.


April 13, 2026

April 15, 2026

April 15, 2026