
April 13, 2026
Explore Memphis detox centers offering discreet care near key neighborhoods and landmarks to support urgent opioid recovery with Trifecta Healthcare Institute.
Start Your Journey NowWritten and reviewed by the clinical team at Trifecta Healthcare Institute, a men’s-only treatment center in Tennessee specializing in substance use, mental health, and dual diagnosis care.
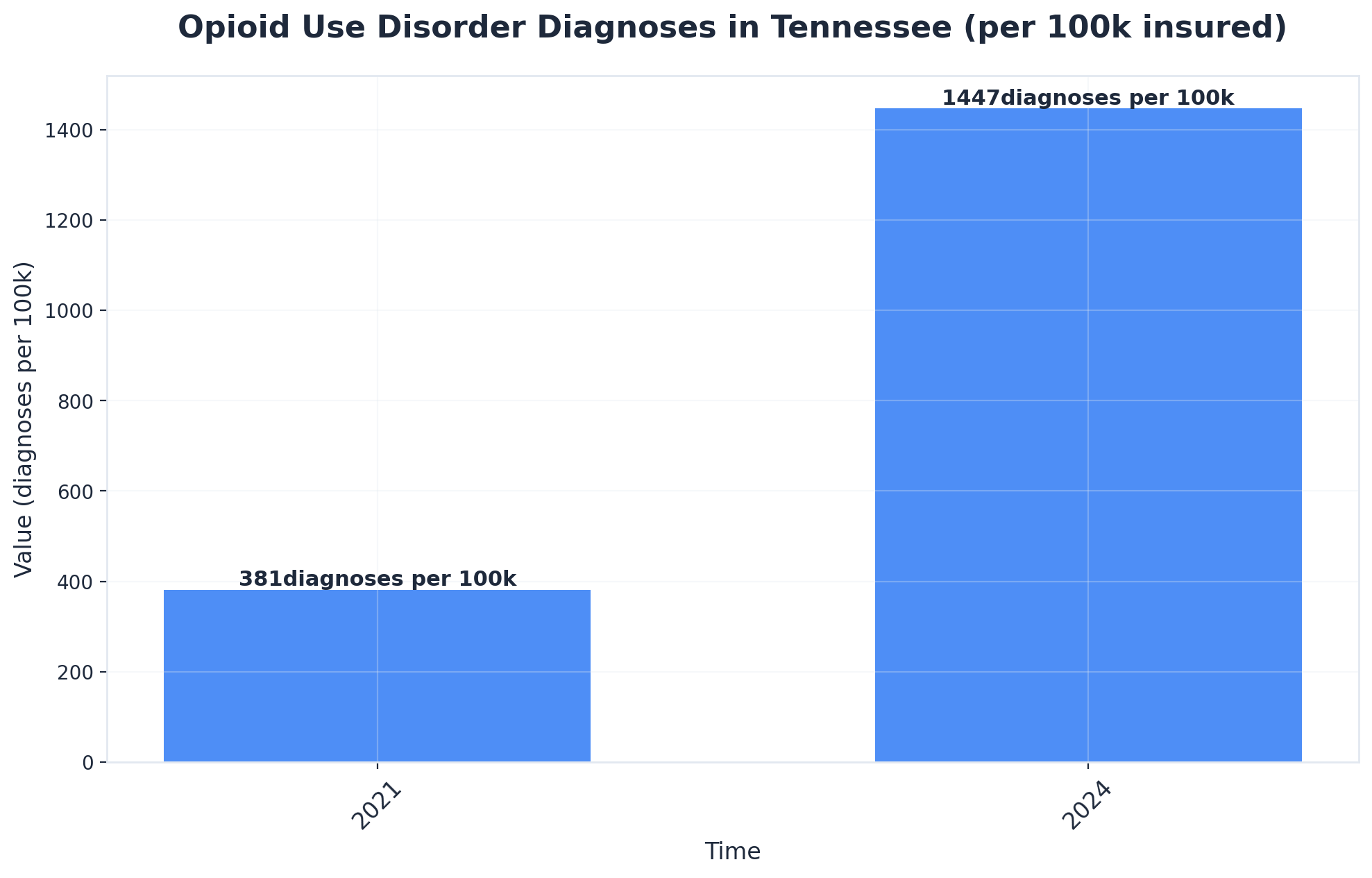
Just south of Shelby Farms and stretching into historic neighborhoods like Cooper-Young and Orange Mound, the effects of Tennessee’s opioid crisis are impossible to ignore for clinical professionals. Memphis—anchored by landmarks such as St. Jude Children’s Research Hospital and Beale Street—sits at the epicenter of a staggering escalation, driving an unprecedented need for high-quality Memphis detox centers. In 2024, Tennessee recorded the highest rate of opioid use disorder diagnoses in the nation: 1,447 per 100,000 insured residents, nearly quadrupling from 381 per 100,000 in 2021.1
This surge has touched every corner of the city, from Midtown and Binghampton to Whitehaven and South Main. For industry peers coordinating care, this intensifies the demand for medically supervised detox and amplifies the local need for rapid, streamlined admissions processes.
"I never thought opioid dependence would reach so many people in my own neighborhood. Getting into detox quickly was a literal lifesaver for my brother."
— A recent family member of a client from Harbor Town
Professionals working in Memphis-area treatment settings frequently cite the strain on resources and the complexity of cases, especially as opioid use disorder impacts men from Downtown all the way to the University District. Local traffic congestion and parking shortages—particularly for facilities near Overton Square or along Poplar Avenue—can add logistical hurdles for case managers seeking immediate support for their clients.
With the crisis escalating, most providers now coordinate with community partners to streamline admissions and offer services accessible via major routes like I-240. The next section explores how fentanyl’s growing presence in the Memphis drug supply has further complicated detox protocols and raised the stakes for clinical intervention.

Fentanyl’s presence in the Memphis drug supply—especially in neighborhoods like Frayser, Raleigh, and South Memphis—has radically changed the landscape for local detox centers. Unlike heroin or prescription opioids, fentanyl is up to 50 times more potent, making overdoses more common and withdrawal symptoms more severe for those entering treatment. This increased potency means that even a small, unintentional exposure can result in a medical emergency, requiring rapid intervention and specialized protocols.2
When logging patient data into electronic health records, professionals often use F11.20 for Opioid Use Disorder. By pressing Enter on these updated intake forms, clinicians trigger specific fentanyl-focused monitoring alerts. Providers near Methodist University Hospital and along Union Avenue report that fentanyl’s unpredictable effects often necessitate longer stabilization periods, more intensive monitoring, and careful medication management.
Standard withdrawal timelines are no longer reliable, as fentanyl’s fast-acting nature can trigger abrupt and dangerous symptom onset. Local clinicians note that men arriving from North Memphis or the Medical District frequently require customized detox plans, particularly if they have co-occurring mental health concerns or polysubstance exposure.2
Memphis detox centers now commonly integrate harm reduction tools—such as fentanyl test strips and naloxone kits—into their intake and transition processes, a response echoed in programs coordinated through the Shelby County Health Department.10
"Detoxing from fentanyl was a completely different experience than what I’d seen with other opioids in my family. The staff were prepared for it, which made all the difference." — Client from East Memphis
As fentanyl drives a new wave of complexity, the next section will examine how Memphis providers adapt medical detox models and protocols to meet these evolving needs.
Just blocks from the Mississippi River and within reach of neighborhoods like Midtown, Binghampton, South Main, and Whitehaven, Memphis detox centers offer two primary medical detox approaches: inpatient and outpatient. Each pathway addresses unique clinical and logistical realities that Memphis-area professionals know well, especially as the city’s opioid crisis intensifies.
Inpatient detox provides 24/7 medical oversight in a secure, structured setting—an approach especially vital for men experiencing severe withdrawal symptoms, co-occurring mental health issues, or histories of relapse. Facilities near the Medical District are equipped for rapid intervention, crucial given the unpredictable effects of fentanyl and polysubstance use now common throughout Frayser and Orange Mound.2
Inpatient programs often appeal to men from the University District or South Memphis who lack stable home environments or face heightened safety risks.
"After my first night in inpatient detox near Overton Park, I finally felt safe enough to focus on recovery—not on what was happening outside." — Client from Cooper-Young
Outpatient detox, by contrast, allows individuals with milder symptoms and strong home support to receive daily medical monitoring while continuing to live at home. This model is commonly accessed by residents in neighborhoods like Harbor Town or Cordova, where family or peer support is readily available.
Outpatient care can be more accessible for those navigating Memphis’s traffic patterns and limited parking, particularly for centers convenient to I-240 or Poplar Avenue. While both pathways are designed to stabilize withdrawal and prepare men for ongoing treatment, research strongly advises against unsupervised home detox due to significant medical risks, especially given the current local drug supply landscape.4
Medication-Assisted Treatment (MAT) has become a central pillar in how Memphis detox centers stabilize men through withdrawal, especially in neighborhoods like South Main, Binghampton, and the Medical District. Facilities near Overton Park and Cooper-Young regularly rely on evidence-based medications to manage acute opioid withdrawal and reduce the risks posed by fentanyl-contaminated supplies.4
MAT protocols are carefully structured, with initial dosing and monitoring often occurring in a clinical setting, followed by ongoing adjustment based on symptom progression and co-occurring mental health needs. The impact of MAT is substantial for Memphis: research indicates a roughly 50% reduction in mortality for individuals with opioid use disorder when agonist medications are part of the detox protocol.7
This is especially relevant in communities like Whitehaven and Midtown, where rapid access to stabilization can be the difference between life and death. Local providers also coordinate with harm reduction programs—many accessible via I-240 or Poplar Avenue—to ensure continuity of MAT upon discharge, reducing the risk of relapse during the critical transition period.
For men who may have transportation or safety concerns, clinics sometimes facilitate home medication delivery or telehealth follow-up, especially in areas with limited parking or high traffic congestion. This focus on MAT integration sets the stage for addressing another major challenge: the high prevalence of co-occurring mental health conditions among men entering care.
Co-occurring mental health and substance use disorders are a defining challenge in Memphis detox centers, especially for men entering care from neighborhoods like Midtown, South Main, Binghampton, and Frayser. Local clinicians routinely encounter individuals whose histories of depression, anxiety, or trauma intersect with opioid or alcohol use—a pattern that complicates withdrawal and stabilization.
Recent data show that roughly 50% of people with a substance use disorder will also experience a mental health disorder during their lifetime, highlighting the urgent need for dual diagnosis expertise in Memphis facilities. It is important for referring professionals to note that while many facilities, including Trifecta Healthcare Institute, excel at treating co-occurring mental health conditions alongside substance use disorder, they do not offer primary mental healthcare as a standalone service.8
This prevalence is visible across the city’s treatment landscape, from the Medical District near Union Avenue to more residential areas like Cordova and Whitehaven. Men coming from Downtown or Orange Mound often report that untreated PTSD, bipolar disorder, or severe anxiety contributed to both the onset and persistence of substance use.
"It wasn’t until I addressed my PTSD in detox near Overton Square that I finally started feeling hope again." — Client from Harbor Town
The complexity of dual diagnosis cases means that Memphis detox centers must be equipped to screen, assess, and begin addressing mental health needs alongside withdrawal management. Without this integrated focus, relapse rates remain high, and transitions to long-term recovery are less successful.8
Integrated treatment approaches are now foundational in Memphis detox centers, especially for men arriving from neighborhoods like Binghampton, Midtown, Whitehaven, and South Main. Facilities near Overton Park and Union Avenue routinely pair medical detox with on-site mental health support, ensuring that withdrawal management and psychiatric needs are addressed simultaneously.
Multidisciplinary teams—often including addiction physicians, therapists, and peer recovery specialists—work directly with clients from areas like Orange Mound and Cordova to develop personalized plans. These plans blend evidence-based therapies, such as cognitive behavioral therapy (CBT) and trauma-informed care, with structured physical activities.
Clients frequently cite the impact of movement-based recovery programming and brotherhood-style support, especially in group settings near places like St. Jude Children’s Research Hospital or accessible via I-240, as critical for building trust and accountability. For example, integrating activities like boxing, jiu-jitsu, or ice baths helps restore neurochemical balance naturally.
"Group hiking near Shelby Farms helped me reconnect with myself and others in ways talk therapy alone never could." — Client from Harbor Town
These integrated models—pairing therapy, medical oversight, and peer support—align with research showing higher retention and lower relapse rates when mental health and substance use needs are addressed together. Next, the discussion will shift to practical considerations for financing detox and ongoing care in Memphis.8
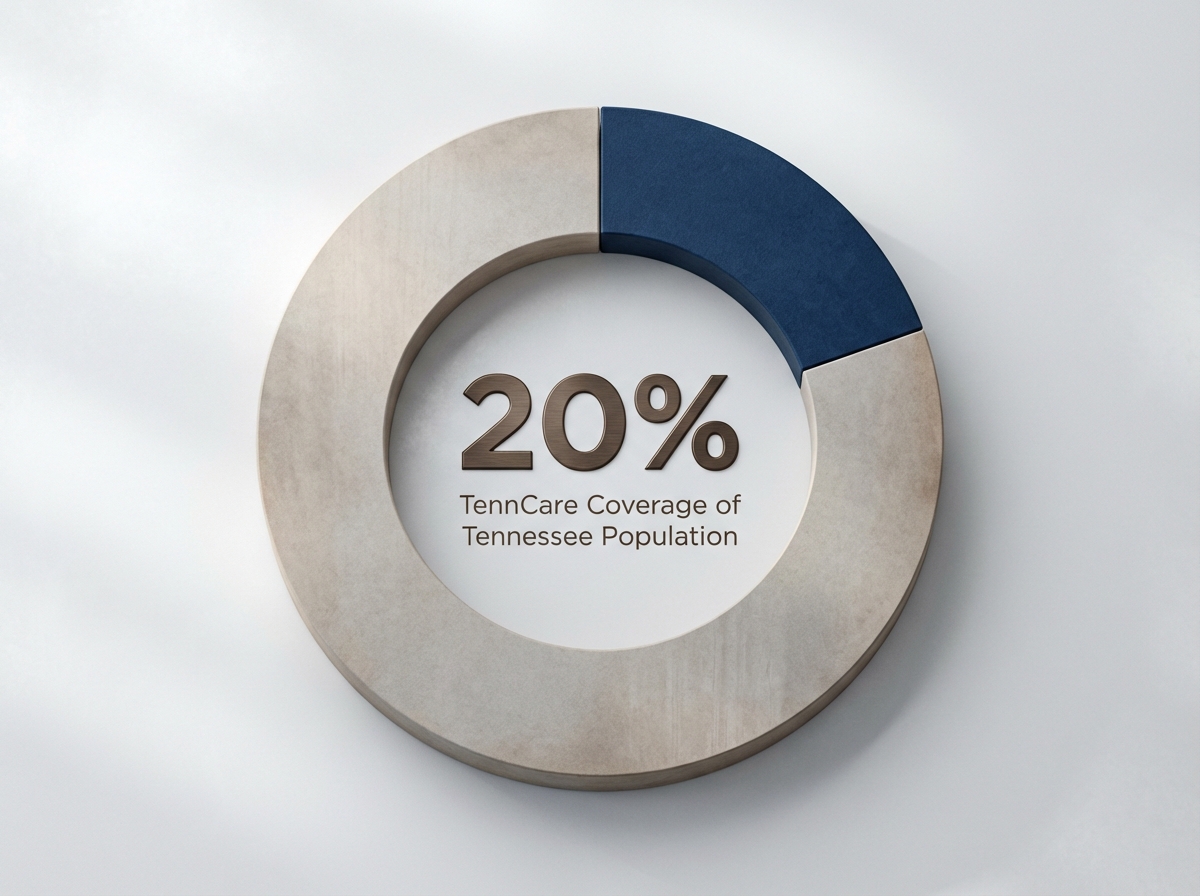
In Memphis, neighborhoods like Midtown, Binghampton, and Whitehaven are home to a diverse population—many of whom rely on TennCare, Tennessee’s Medicaid program, or private insurance to access detox and recovery services. TennCare alone covers about 20% of the state’s population, making it a primary gateway for medically supervised care at Memphis detox centers.6
Facilities near the Medical District, Cooper-Young, and along Poplar Avenue typically coordinate closely with TennCare and major insurers to verify benefits and streamline admissions. This rapid verification process helps clients from South Main to Harbor Town avoid dangerous delays in receiving medical stabilization.
Yet, coverage details and approved providers can vary. Professionals report that some men face hurdles with insurance verification, especially during high-demand periods or when navigating crowded facilities near landmarks like St. Jude Children’s Research Hospital.
Proximity to main routes like I-240 and access to public transportation remain crucial for clients who may need to travel between neighborhoods for intake or follow-up appointments. As insurance and TennCare continue to shape access, understanding these local nuances is essential for ensuring seamless entry into care.6
Understanding the financial landscape of memphis detox centers is essential for professionals coordinating care from neighborhoods like Midtown, Binghampton, Whitehaven, and Cordova. Cost varies significantly based on the level of care and facility location.
Inpatient detox—often located near the Medical District or Overton Park—generally incurs higher expenses. Outpatient detox, accessible in areas like Harbor Town or along Poplar Avenue, is relatively more affordable without insurance.3
Sliding-scale fees and payment assistance are sometimes available, particularly at facilities serving high-need communities in South Main or near the University District. These structures can help reduce barriers for men who may not qualify for TennCare or have gaps in private insurance coverage.
It’s common for professionals to encounter clients whose cost concerns delay or complicate admission, especially when factoring in Memphis-specific challenges like transportation costs or parking fees near busy centers. Analyzing these local cost variables enables more effective care planning and ensures continuity across the treatment continuum.
For professionals guiding male clients through the post-detox continuum, understanding the full spectrum of structured care options significantly impacts long-term retention and clinical outcomes. While detoxification addresses physical dependence, sustainable recovery requires comprehensive programming that rebuilds neurological pathways and behavioral patterns disrupted by prolonged substance use.
Men transitioning from medical detox benefit most from environments that combine evidence-based clinical interventions with active therapeutic modalities designed to restore balance across multiple dimensions of health. Partial hospitalization programs provide the intensive daily structure many counselors and case managers seek for clients requiring high-touch support while beginning real-world integration.
At Trifecta Healthcare Institute's Nashville and Knoxville locations, this phase incorporates individual therapy, group sessions, and trauma processing through EMDR and CBT. This is complemented by movement-based interventions including boxing, jiu-jitsu, and ice baths that regulate stress response systems. These neuroscience-backed physical activities serve as therapeutic tools that naturally restore dopamine and endorphin production, addressing the neurochemical imbalances underlying many relapse patterns.
Intensive outpatient programming offers continued clinical support with increased flexibility, enabling men to rebuild professional and family connections while maintaining therapeutic momentum. This Nashville rehab continuum approach recognizes that neurochemical healing extends far beyond initial detox, requiring sustained intervention to establish new neural patterns and coping mechanisms that support durable recovery outcomes.
Men-only treatment environments create the peer accountability and shared experience that accelerates clinical engagement—a factor consistently correlated with improved retention metrics. When a Knoxville rehab for men combines evidence-based therapies with Trifecta's brotherhood philosophy and active recovery modalities, professionals report stronger client buy-in and measurable improvements in both participation rates and post-discharge stability.
The detox-to-recovery continuum represents one of the most critical clinical frameworks your colleagues can communicate to men in crisis. As peers working across this field, we recognize that medical stabilization addresses only the acute physiological crisis—the neurochemical dysregulation, trauma responses, and behavioral patterns that drive addiction require systematic, graduated intervention.
When you're guiding clients toward appropriate care, understanding how PHP, IOP, and outpatient programming build upon detox outcomes helps establish realistic recovery trajectories and strengthens clinical collaboration from initial contact through long-term maintenance. Trifecta Healthcare Institute's approach to this continuum integrates what many traditional programs overlook: the neurobiological necessity of movement-based interventions alongside traditional therapeutic modalities.
Our men-only environment isn't simply a marketing distinction—it's a clinical framework that leverages accountability dynamics, reduces social performance anxiety, and creates brotherhood connections that function as protective factors during high-risk transition periods. The integration of boxing therapy, jiu-jitsu, ice bath protocols, and outdoor adventure programming directly addresses the dopaminergic and endorphin deficits your clients experience post-detox.
Meanwhile, evidence-based therapies like CBT, DBT, and EMDR process the underlying trauma and cognitive distortions. This dual-pathway model—physical restoration paired with psychological restructuring—produces engagement rates and completion outcomes that inform how we structure referral conversations with families and intervention specialists.
When collaborating with colleagues across Tennessee's treatment landscape, consider how men-specific programming influences clinical outcomes in your own practice areas. The clients who complete structured, gender-responsive continuum care demonstrate measurably different relapse patterns, vocational reintegration timelines, and family reconciliation success compared to those receiving generalized approaches. As professionals committed to evidence-informed practice, our collective impact depends on recognizing that recovery architecture—not just detox access—determines whether men in crisis achieve sustainable transformation or cycle back through emergency services.
When you or someone you love are ready to begin healing—mind, body, and spirit—connect with Trifecta Healthcare Institute. We help men thrive in and out of treatment.
Withdrawal timelines vary based on the substance involved. For short-acting opioids like heroin or illicit fentanyl—both prevalent in Memphis neighborhoods such as Orange Mound and Frayser—withdrawal typically begins 8 to 24 hours after last use and lasts about 4 to 10 days. Long-acting opioids, such as methadone, may trigger symptoms 12 to 48 hours after use, with withdrawal sometimes extending up to 20 days. Alcohol and benzodiazepine withdrawal can start within hours and may persist for a week or longer, requiring strict medical supervision due to risk of severe complications. Local Memphis detox centers structure protocols to match these timelines and ensure safe stabilization for men across Midtown, Binghampton, and South Main.4
Yes, residents of Bartlett and Germantown can access detox services at Memphis detox centers. Many facilities are within a 25-minute drive from these suburbs, with easy access via major routes like I-40 and Poplar Avenue. Local providers frequently coordinate intake and transportation logistics for men coming from neighborhoods such as East Memphis, Cordova, and Collierville as well. This regional accessibility is designed to meet the high demand for medically supervised detox across the broader Memphis metro area, not just within city limits. It’s important for professionals to verify insurance coverage and confirm intake procedures in advance, as capacity and parking availability can vary by location.6
If immediate insurance verification isn’t available, Memphis detox centers typically use a combination of rapid intake protocols and financial triage to prevent delays in care. Facilities near the Medical District or Midtown often provide same-day admissions by confirming eligibility through TennCare or facilitating payment plans while insurance details are processed. Emergency situations or referrals from professionals in Binghampton and South Main may allow for provisional admission, ensuring men aren’t turned away at a critical moment. Staff members regularly help clients from neighborhoods like Cordova or Harbor Town gather documentation, while sliding-scale fees may be offered as a bridge until insurance is verified. Medical stabilization always takes priority in Memphis, with financial arrangements finalized as soon as coverage is confirmed.6
Yes, Memphis detox centers serving neighborhoods like Downtown, Midtown, and East Memphis routinely implement specialized confidentiality protocols for professionals—including physicians, attorneys, and executives—who require discretion. Private intake areas, customized scheduling, and secure parking options near landmarks such as St. Jude Children’s Research Hospital are often available to minimize exposure and uphold privacy. Clinical teams are trained to navigate HIPAA requirements and may coordinate care under initials or aliases when requested. Some facilities in the Medical District and Cooper-Young also offer private rooms or separate group tracks. These steps help ensure professionals can access medically supervised detox while maintaining strict confidentiality, consistent with best practices for privacy in addiction care.4
Memphis detox centers typically coordinate transportation to continuing care—such as PHP, IOP, or sober living—by leveraging partnerships with local transit providers and rideshare services, especially for men transitioning from neighborhoods like Midtown, Cordova, or South Main. Facilities near Overton Park and along Poplar Avenue often arrange shuttle services or work with case managers to secure reliable rides, taking into account city-specific issues like parking scarcity and unpredictable traffic patterns. For clients from areas with limited public transit, staff may help coordinate carpools or provide transit vouchers to ensure continuity of care. These efforts help reduce drop-off rates during this critical handoff.6
Harm reduction programs play a vital connecting role for individuals in Memphis neighborhoods like Frayser, Midtown, and South Main who are at risk for overdose or seeking recovery. The Shelby County Health Department’s initiatives provide free naloxone kits and fentanyl test strips—distributed at community hubs and clinics—to help prevent fatal overdoses and encourage engagement with Memphis detox centers. By meeting men where they are, harm reduction teams build trust and often serve as the first point of contact for those hesitant to access traditional care. These programs partner with local providers along Poplar Avenue and near Overton Park to offer direct referrals, transportation resources, and education about safe detox pathways.10


April 13, 2026

April 15, 2026

April 15, 2026