
April 13, 2026
Explore effective aftercare programs for men that boost recovery through structured support, movement therapies, and peer connection.
Start Your Journey NowWritten and reviewed by the clinical team at Trifecta Healthcare Institute, a men’s-only treatment center in Tennessee specializing in substance use, mental health, and dual diagnosis care.
Critical vulnerability sharply peaks during the first week after completion of formal substance use disorder treatment. For many men, transitioning into structured aftercare programs for men is a decisive crossroads that dictates long-term success.
"Research shows that approximately 74.1% of relapses occur within seven days of discharge, underscoring the need for rapid, structured support during this transition."5
To help you gauge risk and prepare, use this quick checklist for the first week post-treatment:
Anticipating these needs is essential. Without immediate continuity, individuals face heightened emotional, psychological, and environmental triggers. This approach is ideal for those returning to high-risk environments or lacking stable social supports, as structured aftercare reduces the likelihood of impulsive decisions when cravings and stress peak5.
It’s important to recognize that relapse is not a sudden event but a process with warning signs often visible in the first week. By prioritizing proactive engagement, spouses and partners can help reinforce accountability while buffering against isolation and uncertainty3. Looking ahead, understanding chronic condition management frameworks will clarify why sustained recovery requires more than a single intervention.
Substance use disorder is now widely recognized as a chronic condition—a long-term health issue that requires ongoing management, not a one-time solution. In this framework, aftercare programs for men are designed much like the ongoing care provided for diabetes or hypertension. They deliver structured, regular check-ins, behavioral therapy, and community connection to prevent recurrence and strengthen self-management skills7.
| Care Model | Primary Focus | Typical Duration | Expected Outcome |
|---|---|---|---|
| Acute Intervention | Detoxification & Stabilization | 7 to 30 Days | Short-term physical safety |
| Chronic Management | Behavioral Change & Brotherhood | 3 to 12+ Months | Long-term abstinence & stability |
Evidence indicates that combining formal aftercare with weekly mutual-help groups leads to a 90% twelve-month abstinence rate, significantly outperforming either method alone7. For professional partners, this means that supporting a chronic care model can make a measurable difference in long-term outcomes and stability.
Time investment varies: most aftercare frameworks recommend a minimum of three to twelve months of engagement. Financial resource needs range from $0 for mutual-help groups to $500-$1,500+ per month for structured sober living. This strategy suits families aiming for durable recovery, especially when work, stress, or co-occurring conditions pose ongoing challenges. Next, examining the core components of effective programs will help clarify what structures and supports most powerfully sustain progress after initial treatment.
Clinical support and therapeutic continuity form the backbone of effective aftercare programs for men. In this context, therapeutic continuity simply means maintaining ongoing, structured contact with clinical professionals—such as therapists, counselors, or psychiatric providers—after formal treatment ends. Research consistently demonstrates that men who receive regular clinical follow-up and access to behavioral therapies see markedly reduced relapse rates compared to those without this support7.
It is vital to note that facilities like Trifecta Healthcare Institute provide co-occurring mental health treatment alongside SUD support, ensuring that underlying trauma or anxiety is addressed without acting as a primary mental healthcare facility. Arranging first outpatient appointments before discharge and ensuring that all providers are aligned with the treatment plan helps minimize gaps. Telehealth has emerged as a highly effective solution, especially for men balancing employment or facing travel barriers, with studies showing that remote support can yield outcomes comparable to in-person care1.
Resource requirements for clinical aftercare typically include time for weekly or biweekly sessions (often 60–90 minutes), access to licensed mental health professionals, and, when needed, medication management for co-occurring conditions6. Costs can range from $100-$200 per session if paying out-of-pocket, though insurance often covers a significant portion. This path makes sense for men with dual diagnoses, high relapse risk, or those whose recovery environment is unpredictable. Understanding how clinical support connects with peer and social networks will clarify how aftercare programs for men create a comprehensive safety net for long-term success.
Peer connections are a fundamental pillar of aftercare programs for men, providing both accountability and a sense of belonging that clinical support alone cannot replicate. Peer networks—groups of individuals with shared lived experience—offer a unique environment where men support one another through the ups and downs of recovery. Mutual-help integration refers to the formal inclusion of programs like 12-step meetings, men’s process groups, or specialized recovery fellowships as a core feature of aftercare.
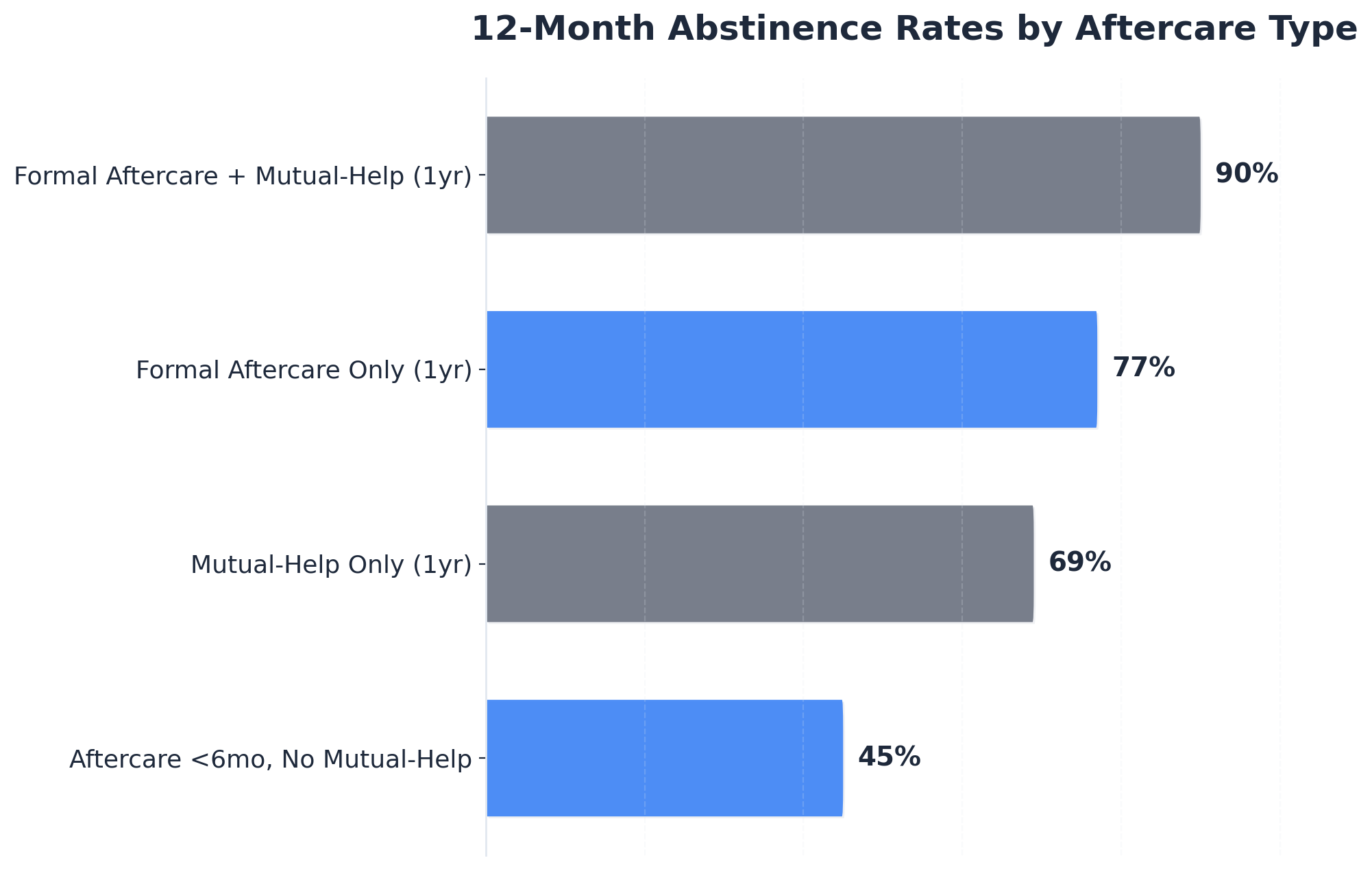
Studies have demonstrated that men combining mutual-help involvement with formal aftercare achieve twelve-month abstinence rates as high as 90%, significantly exceeding outcomes for either approach alone7. In collegiate recovery models, annual relapse rates drop to just 8% when peer support is central8.
Resource needs vary but are generally modest: participation in mutual-help groups is typically free or low-cost, requiring a time commitment of 1–3 hours per week. Alumni and peer-led activities can be scheduled flexibly to accommodate work and family obligations, making this approach accessible for most households. Opt for this framework when your partner responds well to camaraderie, needs ongoing encouragement, or lacks strong sober social ties. Next, movement-based and experiential models will be explored, revealing how physical activity and adventure-based therapies further strengthen aftercare outcomes.
Physical activity functions as more than a wellness add-on in aftercare programs for men—it directly supports neurochemical balance and emotional regulation during recovery. Engaging in exercise triggers the release of endorphins and norepinephrine, which can elevate mood and counteract the neurobiological effects of substance use disorder. Experiential therapies like cold water immersion have gained attention for their rapid impact: research indicates that regular cold exposure decreases cortisol (the primary stress hormone) and boosts endorphin production, with effects lasting up to three hours post-session4.
Baseline State -> Stress Trigger -> Cortisol Spike Intervention -> Ice Bath / Jiu-Jitsu -> Endorphin & Norepinephrine Release Result -> Neurochemical Reset & Craving Reduction If you are researching options online, use search terms like Knoxville rehab for men or Nashville rehab to find programs that prioritize these active modalities. Incorporating movement-based modalities helps rebuild self-efficacy and routine—two factors strongly linked to long-term abstinence. Resource requirements are generally modest: access to safe outdoor spaces, basic equipment, and community or peer support to maintain engagement. Time commitment may range from 30-minute daily walks to 3-5 hours weekly in structured programs, with costs ranging from free outdoor activities to $50-$150 monthly gym fees.
This method works when men feel restless in talk-based therapies or benefit from physical outlets for stress and cravings. Looking ahead, understanding how brotherhood and accountability structures complement physical activity will clarify how aftercare models foster sustained commitment and mutual support.
Brotherhood and accountability structures set movement-based aftercare programs for men apart from more traditional approaches. In this context, brotherhood refers to intentionally fostering a peer community built on trust, shared goals, and mutual responsibility. These environments—such as men’s group training sessions, adventure outings, or alumni meetups—create both camaraderie and a healthy pressure to maintain progress.
Research shows that peer support is among the most powerful and cost-effective elements in aftercare, significantly improving sustained engagement and lowering relapse rates7. For example, men returning to high-stress careers or those managing isolation after treatment often find these structures keep them focused and motivated.
Resource requirements are generally moderate: regular group meetings, access to organized activities, and time set aside for relationship-building. Time commitment typically runs from one to three hours weekly, with costs ranging from $0 to $100 monthly for activity fees, but ongoing engagement is key for lasting benefit. Consider this route if your partner thrives when held accountable by peers or who benefits from a sense of belonging to a group with similar lived experience. Building on these foundations, the next section explores how aftercare programs for men help partners assess and strengthen recovery capital, laying groundwork for lasting stability.
Building recovery capital—the combined personal, social, and community resources that sustain long-term wellness—is a central concept in developing effective aftercare programs for men. Recovery capital includes qualities such as self-esteem, peer relationships, stable housing, and access to meaningful work or activities. Research indicates that greater recovery capital predicts better long-term outcomes, including lower relapse rates and improved quality of life10.
For professionals supporting their partner, this framework offers a practical way to identify gaps, celebrate strengths, and intervene before setbacks escalate. Time investment varies, but regular check-ins (1-2 hours weekly) and collaborative problem-solving sessions can be integrated into existing routines, requiring focused attention rather than significant new financial resources.
Prioritize this when your partner’s journey requires more than just abstinence—such as repairing family dynamics, securing employment, or building new social connections. Next, the discussion turns to structured living and community resources—key supports for men seeking added stability after formal treatment.
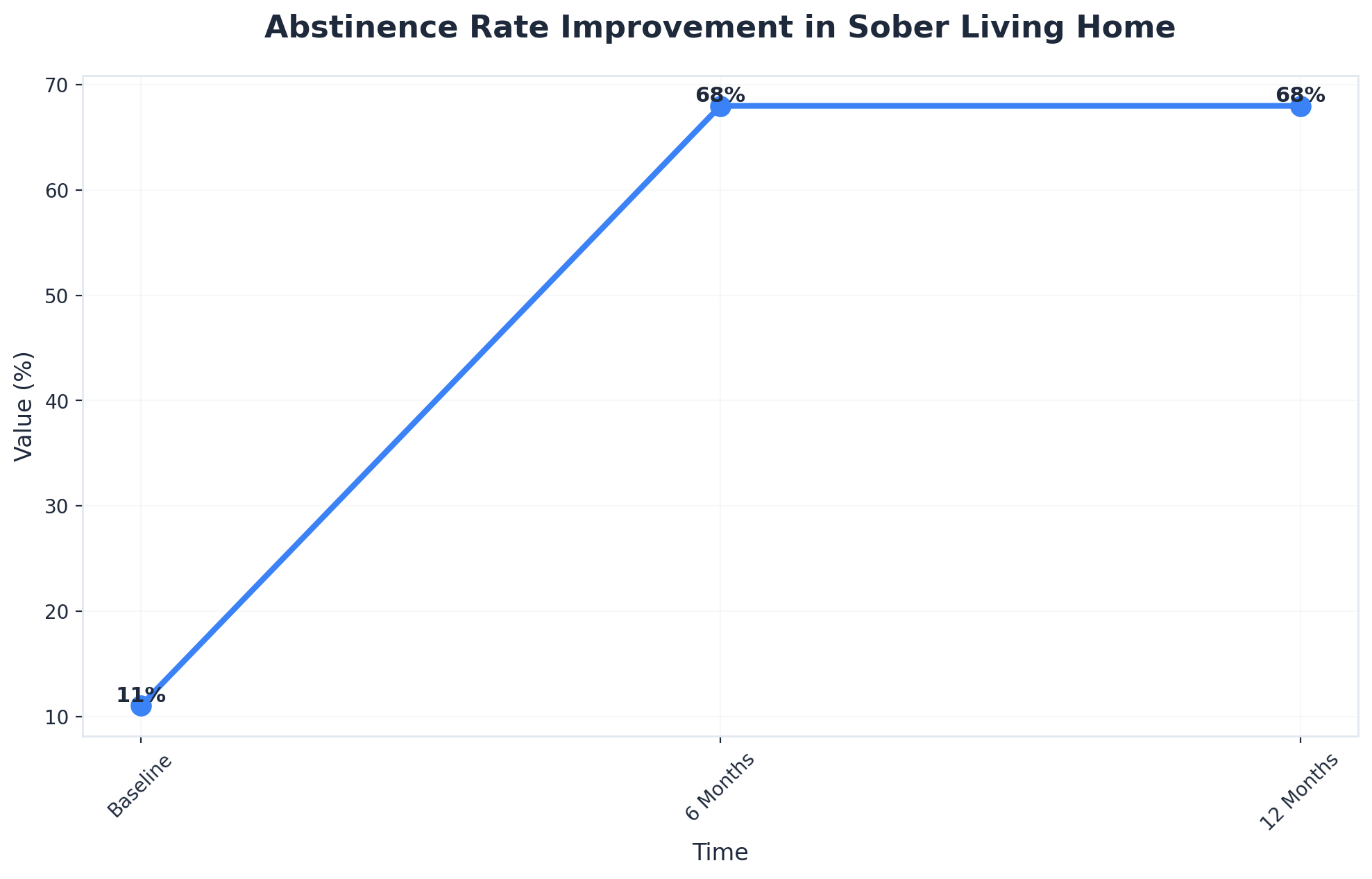
Structured living options—such as sober living homes or recovery residences—provide a stable, substance-free environment that reinforces accountability and daily structure during the high-risk period after treatment. Evidence shows that men residing in such environments see abstinence rates rise from 11% at baseline to 68% at both six and twelve months, alongside reduced arrest rates and improved employment outcomes2.
Community resources—including alumni groups, vocational services, and recreational programs—extend the reach of aftercare programs for men by connecting individuals to broader networks and meaningful activity. While resource demands vary, most structured living environments require shared rent (typically $600 to $2,000+ monthly) and participation in household responsibilities, with time investments ranging from several hours weekly in house meetings to ongoing community engagement.
Community integration activities—such as group outings or service projects—help men develop new social capital and reduce isolation, both powerful predictors of long-term recovery10. This solution fits men who benefit from peer accountability, need to rebuild routines, or face unstable home environments. The next section will address frequently asked questions, clarifying practical concerns about aftercare logistics and family involvement.
If you're wondering what your partner's days will actually look like at a Nashville drug rehab or Knoxville alcohol rehab, here's what to expect. The first 30 days are critical—research shows that this initial month of structured care significantly improves long-term recovery outcomes by establishing new patterns before old habits can reassert themselves. After medical detox stabilizes his physical health, he'll transition into programming designed to address the underlying patterns driving substance use.
His days will include evidence-based therapies—CBT, DBT, and trauma-informed care—combined with movement-based activities that restore neurochemical balance naturally. Mornings might start with boxing or jiu-jitsu, followed by individual therapy sessions that dig into root causes. Afternoons bring group work where men hold each other accountable, building the brotherhood connections that sustain recovery beyond treatment. Ice baths, hiking excursions, and outdoor challenges aren't just physical outlets—they're neuroscience-backed tools that help rewire stress responses and rebuild confidence.
Throughout these 30 days, psychiatric support and medication management address co-occurring mental health conditions alongside substance use disorder treatment. Your partner learns practical skills for managing triggers, processing trauma, and rebuilding daily routines. By month's end, he'll have established healthy patterns, formed meaningful peer connections, and developed tools for the journey ahead—whether continuing in Nashville or Knoxville through an intensive outpatient program (IOP) or transitioning to sober living with ongoing support.
The cost of aftercare programs for men in Tennessee can vary widely depending on the level of structure and clinical involvement. Outpatient aftercare and mutual-help groups are often low-cost or free, while structured sober living homes or intensive outpatient programs may require shared rent or fees for services. Insurance generally covers clinical aftercare components such as therapy, medication management, and outpatient visits, but coverage for sober living or experiential therapies is less consistent1. For men with co-occurring conditions, integrated aftercare supported by insurance can significantly reduce long-term societal costs and improve outcomes1. Always verify benefits directly with providers and insurers.
Deciding between sober living housing and outpatient aftercare alone depends on multiple factors unique to each man’s situation. Sober living is recommended when a partner faces unstable housing, lacks a sober support system at home, or has a history of early relapse after previous treatment. Evidence shows that men in sober living environments achieve much higher abstinence rates—rising from 11% to 68% over twelve months—compared to those without this structure2. Outpatient aftercare may suffice for those with strong family support, a stable home, and established sober routines. This path makes sense when accountability and community are present outside of a residential setting. Individual needs should guide the choice, and consulting with treatment professionals is essential.
Family members play a vital but nuanced role during the aftercare phase. Research highlights the importance of maintaining supportive involvement without crossing into enabling behaviors—such as shielding a partner from natural consequences or micromanaging recovery routines3. Effective support means participating in open, judgment-free communication, encouraging self-responsibility, and respecting boundaries set by aftercare programs for men. Practical strategies include attending designated family support sessions, collaborating on relapse prevention plans, and focusing on encouragement rather than control. This approach supports autonomy and accountability, both shown to reduce relapse risk and help men build sustainable recovery capital10.
Most aftercare programs for men are intentionally structured to support individuals as they return to employment or maintain work commitments. Flexible scheduling, including evening and weekend therapy sessions, as well as telehealth options, allow men to participate in clinical follow-up or peer support while balancing job responsibilities1. Many sober living environments also accommodate shift work and provide transportation resources. This approach works best when clear communication occurs between the aftercare team and the returning employer, ensuring that recovery and professional obligations can be synchronized. For men requiring more tailored support, individualized aftercare planning remains essential to address unique work-life needs1.
Warning signs that an aftercare plan needs adjustment include increased withdrawal or isolation, missed appointments, renewed secrecy around routines, or escalating emotional volatility. Other red flags are a decline in participation with peer or movement-based groups and a return of high-risk behaviors or environments. Research emphasizes that relapse typically unfolds in stages—emotional, mental, then physical—so subtle shifts in mood, motivation, or engagement often precede any actual substance use3. This approach works best when partners monitor for these early cues and proactively communicate concerns, as timely modifications to aftercare programs for men can prevent setbacks and support long-term stability3.
Telehealth and remote support options have become essential components of aftercare programs for men, particularly for those balancing work, family, or living in areas with limited access to in-person services. Studies indicate that remote formats—such as teletherapy and telephone-based continuing care—can deliver outcomes comparable to traditional in-person aftercare, especially when sessions are scheduled regularly and engagement remains high1. The flexibility of telehealth enables consistent accountability and reduces barriers like transportation or time off work. This method works when men require discreet, accessible support or face logistical challenges, but some may still benefit from the camaraderie and structure of in-person groups. The choice should reflect individual needs and preferences, ensuring accountability is maintained in either format.


April 13, 2026

April 15, 2026

April 15, 2026