
April 13, 2026
Learn how to navigate insurance, payment plans, and financial aid to manage the average cost of inpatient rehab effectively and reduce out-of-pocket expenses.
Start Your Journey NowWritten and reviewed by the clinical team at Trifecta Healthcare Institute, a men’s-only treatment center in Tennessee specializing in substance use, mental health, and dual diagnosis care.
The pricing landscape for addiction treatment in 2026 shows a wide spectrum across different levels of care. For professionals guiding men in crisis, understanding the average cost of inpatient rehab is the crucial first step toward securing life-saving care. Residential programs have continued to increase in price over recent years, and this trend is expected to persist1. In contrast, outpatient and intensive outpatient modalities remain less expensive but provide different levels of support and structure.
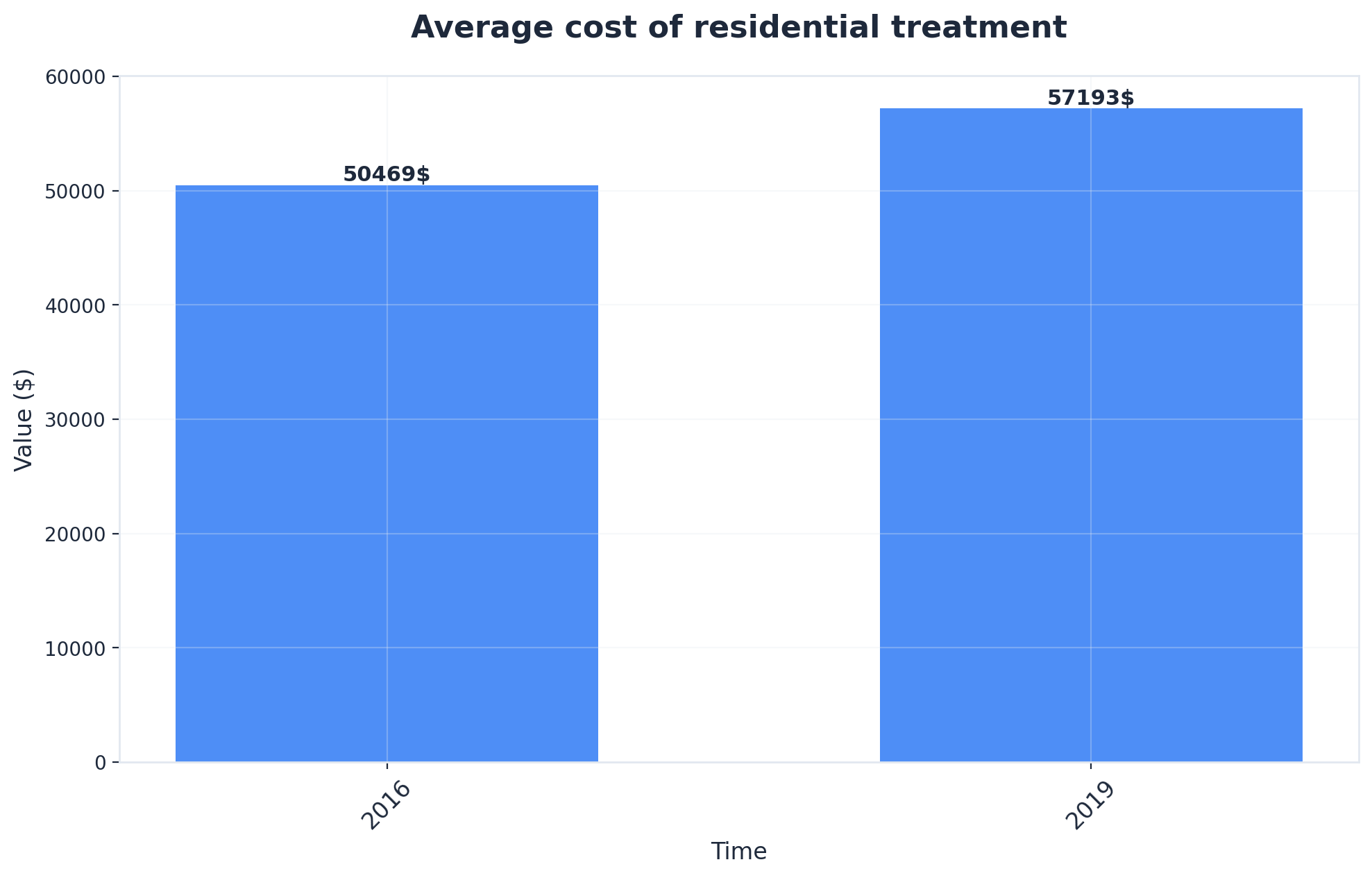
A side-by-side look at current data helps illustrate the range of costs involved when evaluating treatment options:
| Treatment Modality | Estimated Average Cost (2026) |
|---|---|
| Residential (Inpatient) Rehab | $57,193 |
| Therapeutic Community | $20,430 |
| Methadone Maintenance | $5,897 |
| Intensive Outpatient | $1,908 |
| Non-Methadone Outpatient | $1,561 |
This table highlights the significant price difference between round-the-clock residential care and outpatient models, which generally offer more flexibility but less supervision1. It's also important to note the growing demand for specialized programs, such as dual diagnosis or movement-based recovery, which can affect overall costs.
Facilities serving men in Tennessee, especially those embracing neuroscience-backed therapies and peer-driven accountability, may fall into the higher end of the inpatient pricing spectrum. Understanding this landscape allows professionals to guide clients and families toward the most clinically appropriate—and financially sustainable—options. The next section examines the factors driving these ongoing increases in residential treatment costs.
Several forces are fueling the continued rise in the average cost of inpatient rehab, especially for residential programs. Staffing is one of the most significant contributors. Recruiting and retaining highly trained clinical staff, medical personnel, and specialized therapists requires competitive compensation—especially as demand for dual diagnosis and trauma-informed care expands.
"Investing in comprehensive, movement-based residential care upfront often mitigates the long-term financial and personal costs of chronic substance use, providing a solid foundation for sustainable brotherhood and recovery."
Facilities in Tennessee and across the country must also invest in ongoing professional development and compliance training, all of which add to operational expenses1. Facility infrastructure represents another major cost driver. As expectations shift toward more comfortable, therapeutic environments, providers are renovating spaces and adding amenities like private rooms, outdoor activity areas, and specialized gyms for movement-based recovery.
These upgrades are essential for programs that integrate neuroscience-backed activities, but they raise fixed costs substantially1. Increased regulatory oversight and accreditation standards further impact the financial landscape. Meeting state and federal guidelines—particularly for medical detox, psychiatric support, and medication management—requires investments in technology, documentation systems, and quality assurance processes4.
The adoption of innovative therapies, such as EMDR, jiu-jitsu, and ice bath therapy, also requires additional equipment and specialized staff training. These combined factors explain why the average cost of inpatient rehab consistently outpaces inflation, with a 13.28% increase between 2016 and 2019 alone1. Understanding these rising costs helps professionals advocate for reimbursement rates that reflect the true complexity of modern residential care.
When you're in crisis and need immediate help, the last thing you want is to navigate insurance bureaucracy alone. The reality is that getting into medical detox and structured treatment can happen quickly—often within 24 hours—but understanding your coverage shouldn't slow down your path to safety and healing. Most insurance plans cover the full continuum of addiction treatment, from medical detox through movement-based programming and sober living, though coverage percentages vary by level of care.
When verifying benefits through an insurance provider's online portal, professionals may need to input specific diagnostic or billing codes. For example, you might use the search function (often accessed by pressing Ctrl + F) to locate coverage details for:
Billing Code: H0011 (Alcohol and/or drug services; acute detoxification) Billing Code: H0018 (Behavioral health; short-term residential)Trifecta's benefits verification team handles this process for you, conducting a comprehensive investigation of your behavioral health benefits while you focus on the immediate decision to get help. This professional verification examines what's covered under your specific plan—from medical detox and psychiatric support through our evidence-based therapies and movement-based recovery programming including boxing, jiu-jitsu, and outdoor adventure activities.
It is important to note that Trifecta Healthcare Institute specializes in treating substance use disorders with co-occurring mental health conditions. We do not offer primary mental healthcare. Insurance verification must specifically target SUD primary diagnoses with secondary mental health support to ensure accurate coverage estimates.
The team identifies authorization requirements, coverage percentages for our Nashville and Knoxville locations, and potential pathways for maximizing your benefits throughout your entire treatment journey. Rather than spending hours on hold with insurance representatives, men in crisis can connect directly with Trifecta's admissions team, who coordinate benefits verification in real-time.
This approach removes barriers between recognizing you need help and actually receiving it. The verification process examines coverage for our full continuum:
Understanding your coverage matters because it shapes your treatment plan, but it shouldn't delay your admission when you're ready to take action. Most plans provide strong coverage for evidence-based therapies including cognitive behavioral therapy, dialectical behavior therapy, and trauma-focused interventions like EMDR, along with the co-occurring mental health support that addresses underlying conditions alongside substance use disorders.
Trifecta's team specifically investigates whether your plan covers the movement-based programming that distinguishes our approach—the neuroscience-backed physical activities that restore neurochemical balance and provide active alternatives to traditional talk therapy alone. For men whose insurance coverage proves limited or who lack insurance entirely, Trifecta's financial counseling team identifies combinations of available benefits, payment arrangements, and supplementary resources that make comprehensive treatment accessible.
The goal is removing financial uncertainty as a barrier to getting help when you need it most. Whether your plan covers 100% of medical detox or requires cost-sharing for extended residential programming, having a dedicated team navigate these details means you can focus on the decision that matters: committing to your recovery within a brotherhood of men who understand the journey.
This verification process typically completes within hours, not days, allowing for rapid admission to medical detox when you're ready. Trifecta's experience working with Tennessee insurance networks—and understanding the specific nuances of coverage for men's addiction treatment in Nashville and Knoxville—means identifying opportunities for maximizing benefits while ensuring you receive the full continuum of care necessary for sustainable recovery.
Facility-based payment arrangements remain a central tool for addressing the average cost of inpatient rehab, especially as out-of-pocket expenses continue to rise despite insurance coverage gaps1. Many residential treatment centers now offer internal financing structures to help clients and families spread the burden of these costs over time.
Typically, these arrangements allow men entering programs to break large balances into manageable monthly installments. Payment schedules are often customized based on the client’s financial situation, insurance reimbursements, and the length of stay recommended by clinical teams. For professionals coordinating care, it is helpful to clarify early on whether the facility’s payment plan is interest-free, requires a down payment, or includes administrative fees.
Some centers in Nashville and Knoxville may also align payment schedules with the timing of insurance determinations, which can help minimize risk for both parties. The following table summarizes common features of facility-based payment plans:
| Payment Plan Feature | Potential Benefit |
|---|---|
| Monthly Installments | Reduces upfront financial burden |
| Income-Based Adjustments | Increases access for lower-income men |
| Deferred Start Dates | Allows treatment to begin immediately |
| No-Interest Options | Keeps overall repayment manageable |
| Admin Fees/Down Payments | Clarifies true out-of-pocket exposure |
Having transparent discussions about payment plan options empowers clients to engage in residential care without delaying treatment. Next, professionals can look at third-party healthcare financing solutions to further bridge any remaining financial gaps.
Third-party healthcare financing can provide a lifeline for men and families facing the average cost of inpatient rehab when insurance and facility-based plans are not enough. These financing solutions are typically offered by specialized healthcare lenders who work directly with treatment centers, or by national companies with programs designed for medical expenses.
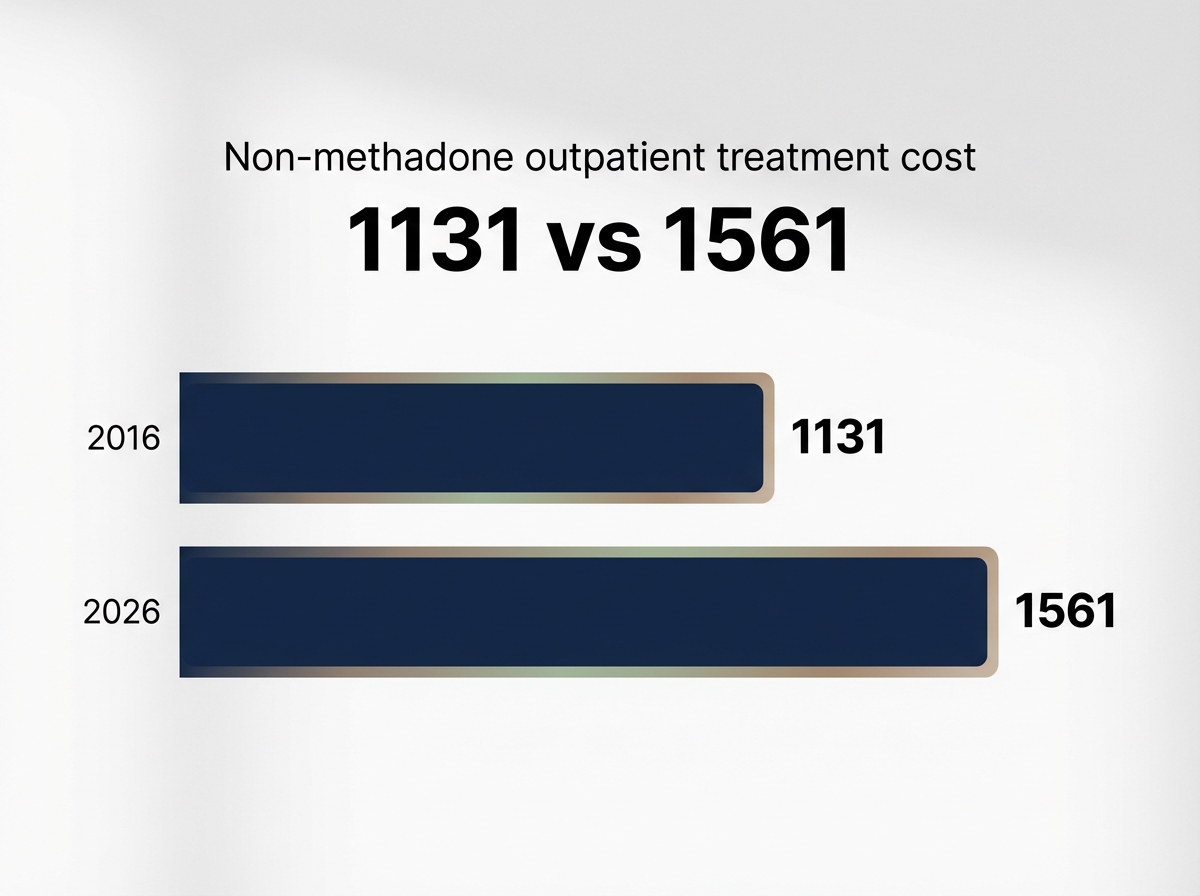
Unlike traditional loans, these options often feature fast application processes and do not always require collateral or perfect credit histories. Financing programs may cover all or part of the upfront balance, allowing clients to start residential treatment without delay. Loan terms can vary significantly, with some offering zero- or low-interest introductory periods, while others set fixed interest rates based on creditworthiness.
For professionals supporting clients in Tennessee, it is useful to compare programs carefully and clarify repayment timelines, as well as any penalties for late payments or early payoff. Some providers integrate automatic payment deductions, streamlining the repayment process and reducing the risk of missed payments.
The table below outlines key features to consider when evaluating third-party financing options for the average cost of inpatient rehab:
| Financing Feature | Consideration for Clients |
|---|---|
| Interest Rate Structure | Impacts total repayment amount |
| Repayment Term Length | Affects monthly payment size |
| Approval Requirements | Determines eligibility |
| Funding Speed | Influences treatment start timeline |
| Payment Flexibility | Supports changing financial situations |
Exploring these options can empower professionals and families to access needed care quickly, even when other resources fall short1. The following step will address how public funding and grant-based resources can further support long-term recovery.
Understanding insurance coverage and funding sources for Nashville rehab or Knoxville rehab for men represents just the first step—comprehensive treatment planning must also account for the continuum of care that extends beyond primary treatment. Men completing intensive programs face the critical transition back to daily life, where maintaining sobriety requires ongoing support structures and accountability systems that may or may not be covered by the same funding mechanisms that paid for initial treatment.

Research consistently shows that individuals engaged in long-term aftercare demonstrate significantly higher success rates than those who disconnect after primary treatment, making it essential to understand how insurance plans, state funding, and facility financing address extended care services. Effective recovery maintenance involves multiple components working together within Trifecta's brotherhood model.
Alumni services provide continued connection to peers who understand the journey firsthand—including monthly alumni gatherings, peer mentorship programs pairing recent graduates with men further along in recovery, and 24/7 access to alumni support networks during moments of crisis. Structured sober living environments in Nashville and Knoxville establish peer accountability during the vulnerable early months of independence, with house meetings, random drug screening, and shared responsibility systems that reinforce the brotherhood philosophy developed during treatment.
Outpatient programs offer flexible scheduling that accommodates work and family responsibilities while maintaining therapeutic engagement, though men should note that while many insurance plans cover primary PHP and IOP services, extended alumni programming and sober living costs often require out-of-pocket payment or alternative funding arrangements. Movement-based recovery programming continues playing vital roles in sustained wellness beyond initial treatment.
Trifecta's specific approaches—including boxing therapy for emotional release, jiu-jitsu for discipline and focus, ice baths for neurochemical regulation, hiking through Tennessee landscapes, and outdoor adventures like white-water rafting—become lifelong tools rather than temporary interventions. Alumni maintain access to these activities through ongoing programming, with regular boxing sessions, group hikes, and adventure outings that keep men connected to the physical practices that helped restore neurochemical balance during treatment.
These evidence-based movement therapies support stress management and emotional regulation as men build fulfilling lives grounded in recovery principles, brotherhood accountability, and the active engagement that distinguishes Trifecta's approach to long-term healing.
If insurance denies coverage after treatment has started, professionals should respond quickly to protect clients from unexpected financial exposure. Begin by requesting a detailed explanation of the denial in writing. Many insurance plans are required to provide clear reasons and outline the appeals process, particularly for behavioral health services 4. Providers can gather supporting documentation—such as clinical notes and medical necessity letters—to strengthen an appeal. While the appeal is underway, treatment centers may offer short-term payment plans or help clients apply for public funding or grants to offset the average cost of inpatient rehab 1. Communication and advocacy are key to minimizing disruption in care.
Family members and employers can help cover the average cost of inpatient rehab, but tax implications depend on how the funds are provided. Direct payments by a family member to the treatment facility are generally not considered taxable gifts under IRS rules, which allows for larger contributions without penalties. Employers may offer Employee Assistance Programs (EAPs) or direct financial support, but these benefits could be taxable income unless structured as a qualified medical expense or under a health plan 4. Professionals should encourage clients to consult with a tax advisor to ensure contributions are handled appropriately and avoid any unexpected tax burdens.
Residential program costs vary by length, with longer stays typically resulting in higher total expenses but sometimes a lower cost per day. For example, the average cost of inpatient rehab for a standard 30-day program is a significant investment, but 60- and 90-day options generally multiply the base rate by two or three, respectively, with occasional discounts for extended stays 1. Longer durations may provide greater clinical benefit for men with complex substance use or co-occurring mental health needs, making the higher up-front cost worthwhile from a recovery perspective. Professionals should review each facility’s pricing structure, as some Tennessee providers offer bundled rates or sliding scale adjustments for longer commitment periods. Comparing program lengths helps clients and their support teams balance clinical outcomes with financial sustainability.
Many Tennessee addiction treatment facilities do offer income-based sliding scale options to help make the average cost of inpatient rehab more accessible for men with limited financial resources. Sliding scale arrangements adjust the total out-of-pocket cost according to a person’s household income, family size, and ability to pay. This approach allows professionals to connect clients with quality care while minimizing financial barriers.
Eligibility for sliding scale programs typically requires documentation, such as recent pay stubs, tax returns, or public benefits statements. Facilities may also prioritize applicants who do not qualify for Medicaid or have exhausted private insurance benefits. Because funding and policies can vary, it’s helpful to contact each facility directly to confirm program availability and application procedures 1. Using sliding scales alongside public resources enables more men to begin medically supervised detox and structured recovery, even if their initial means are limited.
Veterans seeking help with the average cost of inpatient rehab can access several dedicated financial assistance options. The U.S. Department of Veterans Affairs (VA) is the primary resource, offering coverage for inpatient substance use disorder treatment at VA facilities and, in some cases, through community care partners when local VA programs are unavailable 4. Veterans must typically enroll in VA health benefits and complete a clinical assessment to determine eligibility and the appropriate level of care. Some state and local grants further supplement VA coverage, especially for men with service-connected disabilities or those experiencing housing insecurity. Professionals should encourage veterans to work closely with VA case managers, as they can help coordinate benefits and facilitate access to specialized residential programs that meet both mental health and substance use needs 1.
Stepping down from residential to outpatient care can have a major impact on the overall treatment costs for men with substance use disorders. Residential programs are the most expensive due to 24/7 supervision, medical support, and integrated therapies. By transitioning to an outpatient or intensive outpatient program, clients typically see a sharp reduction in weekly or monthly expenses. For example, national data shows the average cost of inpatient rehab is much higher than the average cost of outpatient services, sometimes by a factor of 20 or more 1. Outpatient care still offers structure and accountability but is designed to fit around work, family, and community responsibilities. This step-down approach helps maintain clinical progress while easing financial strain, especially for those who have exhausted insurance benefits or public funding options.


April 13, 2026

April 15, 2026

April 15, 2026