
April 13, 2026
Learn how TennCare covers therapy services, eligibility criteria, and treatment options across Tennessee for behavioral care by Trifecta Healthcare Institute.
Start Your Journey NowWritten and reviewed by the clinical team at Trifecta Healthcare Institute, a men’s-only treatment center in Tennessee specializing in substance use, mental health, and dual diagnosis care.
When professionals in the addiction treatment sector ask, does TennCare cover therapy, the answer is rooted in Tennessee’s evolving Medicaid framework. Facing a unique regional challenge—where opioid-related hospitalizations in East Tennessee remain disproportionately high—the state has structured its behavioral health benefits to address acute needs across diverse populations, from the urban core of Memphis to the rural reaches of the Upper Cumberland.
The program covers outpatient therapy (individual, group, and family), crisis intervention, medication management, and specialized substance use disorder services. Notably, TennCare emphasizes evidence-based modalities: cognitive behavioral therapy (CBT), dialectical behavior therapy (DBT), trauma-informed care, and medication-assisted treatment (MAT) are part of its core offerings for both adults and youth.3,5,9
For clinical teams guiding men toward a Nashville rehab environment, TennCare covers medical detoxification, intensive outpatient programs (IOP), and residential services aligned with American Society of Addiction Medicine (ASAM) criteria, ensuring access to gold-standard treatment approaches. The Buprenorphine Enhanced Medication-Assisted Recovery and Treatment (BESMART) program, available statewide, increases access to MAT for opioid use disorder—a critical need in regions like East Tennessee.5,6
"State regulations require all covered therapies to meet strict definitions of medical necessity, with clinical decisions grounded in recognized standards and reviewed by licensed professionals." — Tennessee Department of Mental Health and Substance Abuse Services
For professionals working in Tennessee, the answer to the question regarding therapy coverage is unequivocally yes—provided the services are evidence-based and medically necessary. The next section explores how these services are delivered through Tennessee’s managed care structure.
TennCare’s behavioral health services are delivered through three Managed Care Organizations (MCOs): Amerigroup, BlueCare, and UnitedHealthcare Community Plan. Each MCO contracts with a network of providers, allowing members in regions spanning from Nashville to Chattanooga and Memphis to the Tri-Cities to access outpatient therapy, medical detox, and substance use disorder treatment within their local communities.3
The MCO structure, established statewide in 2009, was designed to improve care coordination by integrating physical and behavioral health services under a single administrative umbrella. This integration is especially relevant for men in recovery who often present with both substance use and co-occurring mental health conditions.
Under this framework, each MCO is responsible for utilization management, network adequacy, and ensuring timely access to evidence-based therapy. State oversight holds MCOs accountable for meeting performance benchmarks, such as maintaining adequate provider networks and reducing wait times. Despite the presence of managed care, Tennessee’s chronic behavioral health workforce shortage—impacting both urban centers like Knoxville and rural stretches of the Plateau—directly affects real-world access to therapy and SUD treatment.8
The challenge of behavioral health workforce shortages in Tennessee is acute and deeply regional. Data from recent state reports show that Tennessee ranks 46th in the nation for mental health provider availability, with just one provider for every 560 residents, compared to the national average of one per 340. This deficit is even more pronounced outside of major metros.2
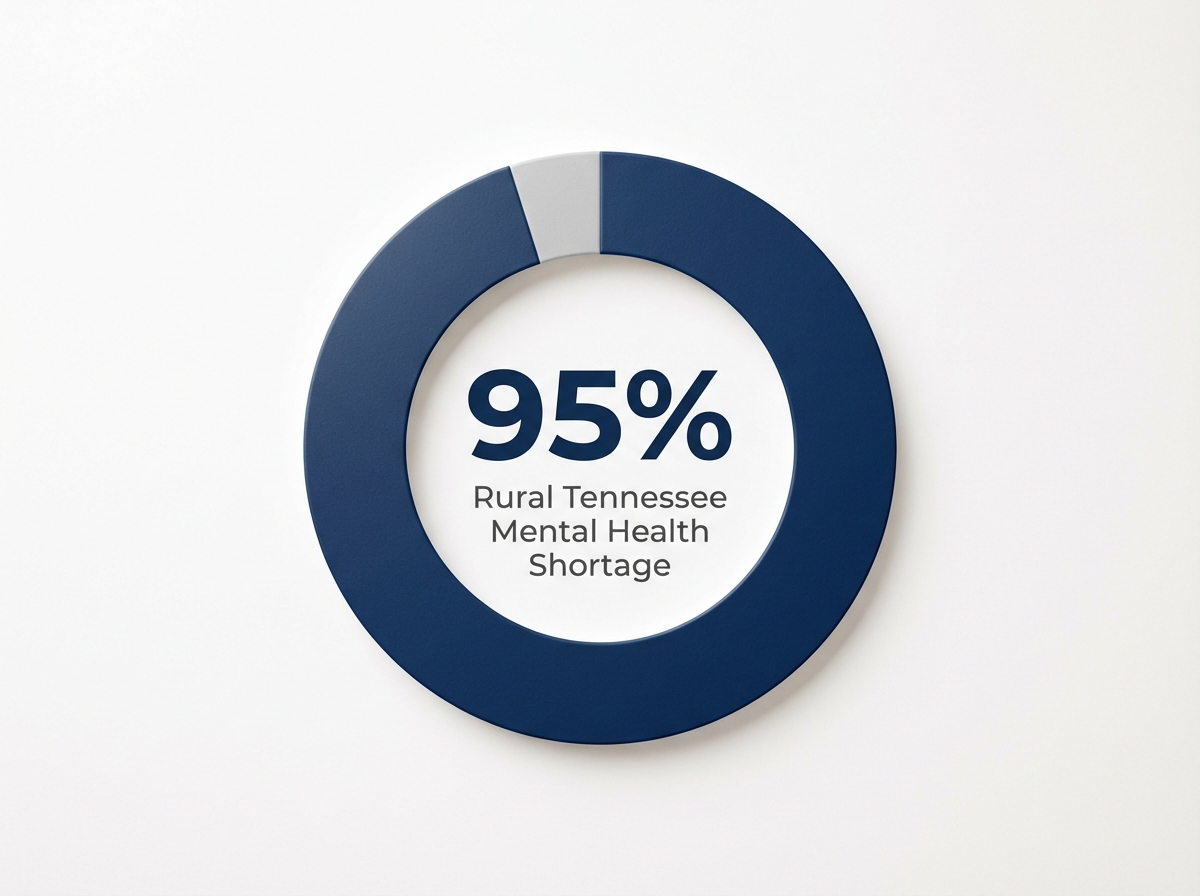
In rural stretches of West Tennessee, the Plateau, and the Upper Cumberland, 95% of counties are federally designated as Mental Health Professional Shortage Areas, reflecting the stark maldistribution of clinicians. Urban centers like Nashville and Knoxville have more robust networks, but even there, wait times and provider scarcity remain persistent concerns for clinical teams trying to place men in immediate care.1
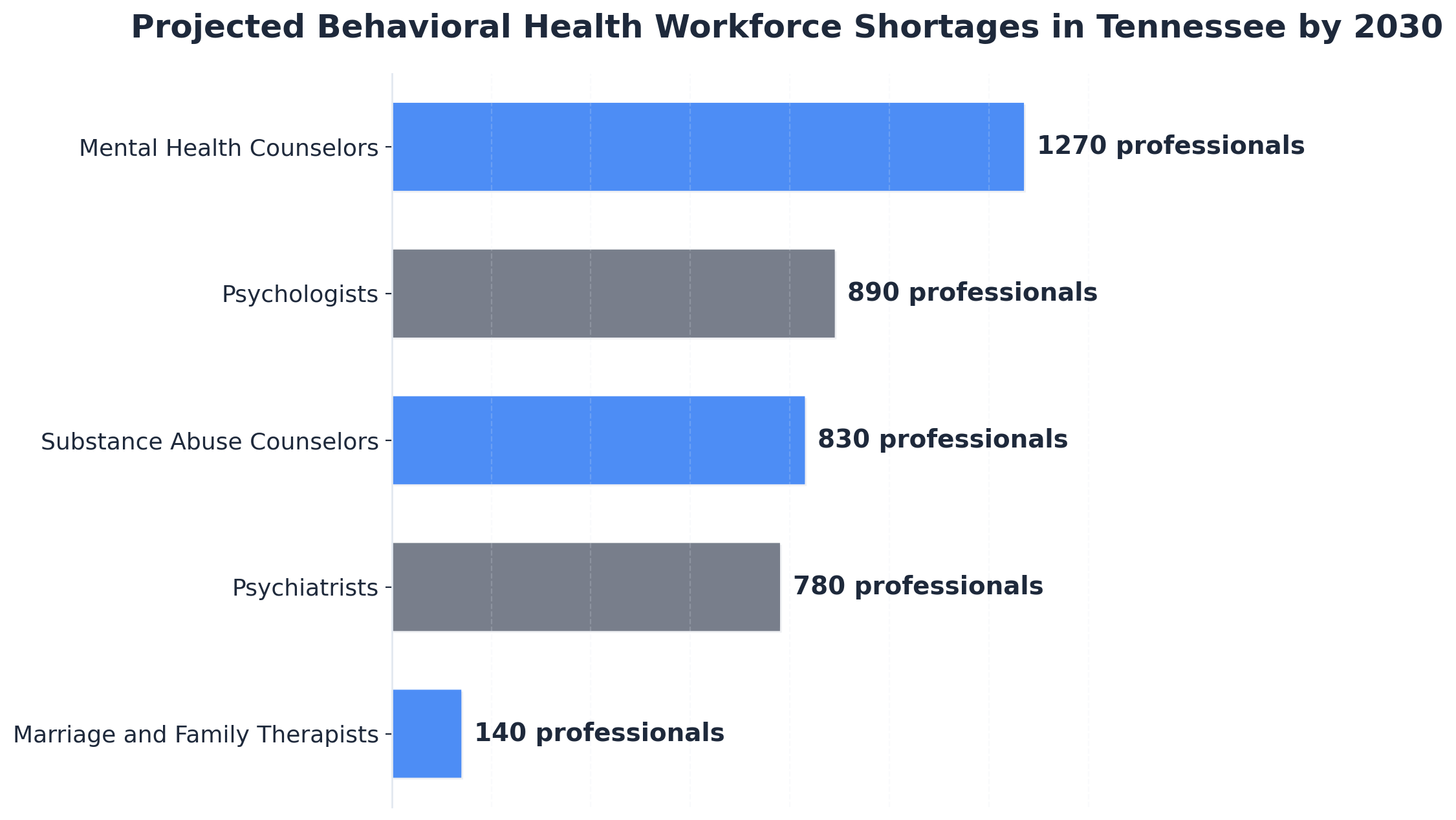
For men seeking substance use disorder treatment or co-occurring mental health support under programs like TennCare, these shortages translate to real-world delays and barriers. Projections indicate that by 2030, Tennessee will face deficits of over 1,200 mental health counselors, nearly 900 psychologists, and close to 800 psychiatrists statewide. Community behavioral health organizations across the state report that 97% are struggling to recruit new staff, and over 60% are dealing with growing patient waitlists.2
Several interconnected systemic and economic barriers drive Tennessee’s behavioral health provider shortage, directly impacting whether TennCare members can access therapy in a timely manner. The most cited root causes include:2
Student loan debt also plays a role, with high educational costs and limited state loan forgiveness options until recent years. This financial disincentive discourages both new graduates and experienced providers from practicing in the state or remaining in the sector long-term, especially in regions like the Plateau or rural West Tennessee.
While the foundational coverage exists, these entrenched barriers mean that coverage alone does not ensure access. Tennessee’s efforts to expand the workforce through scholarship programs and retention bonuses reflect growing recognition of these challenges.2
Telehealth and mobile health services have become essential tools for addressing Tennessee’s persistent gaps in behavioral health access, especially in the wake of critical workforce shortages and pronounced rural disparities. Since 2020, state-backed telehealth initiatives have enabled TennCare members across Tennessee—from the Panhandle and the Upper Cumberland to Memphis and Knoxville—to connect with licensed therapists and addiction specialists virtually, reducing travel and wait times.1
Community mental health centers now widely integrate secure video platforms to deliver therapy sessions, crisis intervention, and follow-up care. These services are particularly vital for men seeking substance use disorder treatment in regions where provider shortages are most severe. For professionals guiding men toward a Knoxville rehab for men, telehealth bridges the gap during the critical window between detox and residential admission.
To verify telehealth eligibility within the state's provider portal, administrative staff often use specific diagnostic and billing codes. For example, verifying a co-occurring disorder might require querying the system:
Mobile health clinics, such as those deployed through Project Rural Recovery, bring integrated behavioral and physical health care directly to underserved counties. In 2023, four mobile units provided services across 20 rural Tennessee counties, offering therapy, medication management, and screening on-site. This model has proven especially effective for engaging individuals who face transportation barriers or are hesitant to seek care in traditional clinic settings.1
The Buprenorphine Enhanced Medication-Assisted Recovery and Treatment (BESMART) program stands out as a targeted response to Tennessee’s opioid epidemic, offering a specialized provider network for TennCare members diagnosed with opioid use disorder. BESMART providers—found from Memphis and Nashville to the Tri-Cities—benefit from enhanced reimbursement rates and access to expanded buprenorphine formularies, supporting more flexible dosing protocols than typical Medicaid plans.
Streamlined prior authorization and care coordination through BESMART help accelerate treatment initiation, a crucial factor given Tennessee’s high rates of opioid-related hospitalizations, particularly in East and Northeast Tennessee. For men seeking recovery, BESMART’s focus on rapid access to medication-assisted treatment addresses both the clinical urgency of opioid dependence and the practical barriers created by provider shortages.6
The program’s model supports continuity of care, often bridging inpatient detox with outpatient therapy and peer support, which is essential for long-term recovery in the state’s diverse communities. For professionals evaluating whether TennCare covers therapy in opioid use disorder care, BESMART demonstrates that the answer is yes—and that innovative, regionally attuned programs can make that coverage actionable.6
Tennessee’s regulatory framework for behavioral health hinges on a clear, enforceable definition of medical necessity, which governs all therapy coverage decisions under TennCare. The state’s administrative rules (specifically Rule 1200-13-16-.02) mandate that a covered service must be recommended by a licensed provider, required to diagnose or treat a specific condition, proven safe and effective, and be the least costly effective alternative—mere convenience for the individual or provider does not qualify.10
These criteria apply equally to therapy modalities, whether in a Nashville rehab or a Knoxville rehab for men, and serve as the clinical threshold for prior authorization and continued care reviews. In practice, Managed Care Organizations (MCOs) conduct utilization reviews to assess whether therapy requests meet these standards before authorizing sessions.
Utilization review is performed by behavioral health professionals, and determinations are subject to appeal and oversight by the state. This system is designed to ensure that coverage for therapy is both medically justified and consistent across Tennessee’s diverse regions, from the Tri-Cities to the Memphis metro area.
Mental health parity laws are central to how Tennessee regulates behavioral health coverage, aiming to ensure that therapy and addiction treatment benefits are offered on par with medical and surgical care. Tennessee enforces both federal Mental Health Parity and Addiction Equity Act requirements and its own state-level parity mandates.
State statute requires that medical necessity reviews for behavioral health be conducted by clinicians in the same field as the treating provider. Furthermore, a minimum of 12 outpatient behavioral health visits must be approved annually before further review is triggered, ensuring baseline access for men in early recovery.7
For TennCare, this means therapy coverage—including outpatient visits and substance use disorder treatment—cannot be subject to stricter limits or higher barriers than comparable physical health services. Despite these protections, enforcement remains a work in progress. Concerns persist about non-quantitative treatment limitations, such as prior authorization and network adequacy, which can still impede timely access to therapy in major metros like Nashville or in rural communities across the Plateau.7

Men in active crisis facing substance use disorders rarely arrive with addiction alone—underlying mental health conditions like depression, anxiety, PTSD, and unresolved trauma intertwine with dependency, creating interconnected patterns that demand immediate, comprehensive intervention. The first critical step is medically supervised detox, providing the physiological stabilization necessary to address both conditions safely. Without this foundation, attempting to treat co-occurring disorders while the body remains in acute withdrawal proves ineffective and potentially dangerous.
Trifecta Healthcare Institute does not offer primary mental healthcare; rather, we specialize in treating co-occurring mental health conditions alongside substance use disorder. Integrated treatment approaches recognize this interconnection by addressing substance use and mental health simultaneously from the moment detox begins and continuing throughout the recovery continuum. Rather than treating these as separate issues requiring disconnected care plans, integrated models weave evidence-based therapies together within a unified framework.
Nashville rehab programs specializing in dual diagnosis treatment utilize modalities like Cognitive Behavioral Therapy (CBT) to help men identify thought patterns contributing to both mental health symptoms and substance use. Dialectical Behavior Therapy (DBT) builds emotional regulation skills essential for managing co-occurring conditions, while EMDR therapy addresses traumatic experiences that often underlie both disorders. These evidence-based approaches work synergistically when delivered by providers trained in treating the full clinical picture.
The advantage of integrated care extends beyond clinical efficiency—it creates the foundation for sustainable peer support. Trifecta's brotherhood model recognizes that men facing similar co-occurring challenges reinforce clinical work through shared experience and mutual accountability. When men understand they're not alone in navigating interconnected substance use and mental health issues, the isolation that fuels both conditions begins to dissolve.
For men seeking Knoxville rehab for men or Nashville-based programs, integrated treatment eliminates the burden of navigating multiple disconnected systems. This comprehensive foundation proves essential for the movement-based recovery programming—such as boxing, jiu-jitsu, and ice baths—that serve as powerful biohacking tools to restore neurochemical balance and transform crisis intervention into lasting transformation.
The integrated treatment foundation established through medical detox and dual diagnosis care creates the clinical stability necessary for sustainable recovery work. For men in acute crisis, thinking about "months and years" can feel overwhelming—which is why Trifecta's structured continuum breaks recovery into manageable phases. Medical detox addresses immediate physical dependence, PHP stabilizes mental health and builds coping skills, and transitional programming gradually reintegrates men into independent living.
Sober living environments provide the critical middle ground, offering peer accountability through Trifecta's brotherhood model while men rebuild life skills and establish healthy routines within Nashville and Knoxville recovery communities. Alumni services and aftercare programming maintain therapeutic momentum after formal treatment concludes, with the brotherhood philosophy extending far beyond discharge.
Men who trained together during treatment often continue meeting for boxing sessions or jiu-jitsu practice, creating accountability partnerships rooted in shared experience. Regular check-ins, peer support groups, and continued access to recovery coaching help men navigate challenges as they reintegrate into work, family, and community roles. This men-only peer network—built on mutual respect rather than judgment—significantly reduces relapse risk during vulnerable transition periods.
Movement-based activities remain powerful long-term recovery tools precisely because they address neurochemical restoration. Men who establish consistent practices—boxing for dopamine regulation, jiu-jitsu for focus and discipline, ice baths for stress resilience—develop healthy alternatives to substance use while reinforcing the biohacking approaches introduced during treatment. Trifecta recognizes that recovery unfolds over months and years, ensuring men develop resilience and skills necessary for lasting transformation within a brotherhood committed to mutual accountability and growth.
When you or someone you love are ready to begin healing—mind, body, and spirit—connect with Trifecta Healthcare Institute. We help men thrive in and out of treatment.
Uninsured Tennesseans who do not qualify for TennCare have several state-supported options for accessing therapy and behavioral health services. The Behavioral Health Safety Net (BHSN) is the primary resource, providing outpatient therapy, medication management, and peer support to adults meeting income guidelines in all 95 counties—including via telehealth if no local provider is available. Community mental health centers in major metros like Nashville and Knoxville also offer sliding-scale fees or grant-funded services. Rural regions benefit from mobile clinics and telehealth outreach supported by the Department of Mental Health and Substance Abuse Services. While the question "does TennCare cover therapy" is focused on insured populations, BHSN and related programs help fill critical gaps for uninsured residents.1,4
Typical wait times to see a behavioral health provider in Tennessee vary widely depending on region and provider type. In major metros like Nashville and Knoxville, patients often wait several weeks for an initial therapy appointment, while in rural areas—including the Upper Cumberland and the Plateau—waits can extend to several months due to the state’s critical workforce shortage. Recent data show that over 60% of Tennessee’s community behavioral health organizations are managing growing patient waitlists, with 97% reporting difficulty recruiting new staff. While the question of "does TennCare cover therapy" is answered by robust benefits, actual access is shaped by these workforce realities. Telehealth and mobile clinics have helped shorten waits somewhat, especially in underserved regions.1,2
Yes, TennCare members can access therapy providers in both Nashville and Knoxville, provided the provider is in-network with the member’s Managed Care Organization (MCO). TennCare’s behavioral health coverage operates statewide, so members living in one metro area—like Nashville—may receive authorized therapy services in another, such as Knoxville, if the provider participates in their MCO’s network. This flexibility helps address gaps, especially for those who may travel for work or access specialized care not available locally. However, actual availability depends on regional provider networks, and ongoing workforce shortages in Tennessee can still impact wait times and appointment access in both cities.2
If a Managed Care Organization (MCO) denies coverage for recommended therapy sessions under TennCare, members have the right to appeal the decision. The appeals process begins with requesting a reconsideration from the MCO, which must review the case and provide a written explanation. If the denial is upheld, members can file a state fair hearing request through TennCare for an independent review. These rights apply statewide, whether the therapy is sought in Nashville, Knoxville, or rural counties. While "does TennCare cover therapy" is answered affirmatively, denials must meet strict standards of medical necessity and state regulations.10
TennCare covers therapy approaches that are evidence-based, medically necessary, and delivered by licensed professionals, including modalities such as cognitive behavioral therapy and trauma-informed care. While movement-based therapy—like boxing or hiking integrated into clinical treatment—is gaining traction in Tennessee, coverage depends on whether the approach is recognized as evidence-based and is part of an approved treatment plan. Providers must demonstrate that these activities are essential for diagnosis or treatment and not solely for recreation. For professionals considering "does TennCare cover therapy" with movement-based elements, approval is possible if the approach is clinically justified and meets all medical necessity criteria.3,10
TennCare members are not subject to statewide geographic restrictions on which providers they can see, but they must use providers who are in-network with their Managed Care Organization (MCO). This means a member in Memphis can access therapy in Nashville or Knoxville if the provider participates in their MCO’s network. However, actual choice is shaped by regional provider availability, which remains limited in many rural and Plateau counties due to Tennessee’s ongoing workforce shortage. Telehealth has expanded cross-regional access, allowing more members to connect with licensed clinicians regardless of location. For professionals, the answer to "does TennCare cover therapy" includes flexibility in provider location, but real access depends on both network participation and regional workforce capacity.1,3
Tennessee’s behavioral health workforce shortage presents unique obstacles for men seeking substance use disorder treatment. With the state meeting only 15% of its need for psychiatrists and projecting a deficit of 1,270 mental health counselors by 2030, men in need—especially in rural or Plateau regions—often face long waits, fragmented care, and limited access to therapy or medical detox. This gap increases the risk of relapse during critical early recovery, particularly for those requiring integrated dual diagnosis support. While the answer to "does TennCare cover therapy" is yes, the practical availability of evidence-based, male-focused SUD treatment is constrained by these persistent workforce challenges.1,2


April 13, 2026

April 15, 2026

April 15, 2026