
April 13, 2026
Explore how men's outdoor therapy fosters lasting sobriety through movement, peer support, and proven recovery strategies tailored to your goals.
Start Your Journey NowWritten and reviewed by the clinical team at Trifecta Healthcare Institute, a men’s-only treatment center in Tennessee specializing in substance use, mental health, and dual diagnosis care.
Physical activity serves as a direct intervention for repairing the neurochemical imbalances that underpin addiction, making men's outdoor therapy a cornerstone of effective treatment. For men in structured recovery, aerobic movement and strength-based exercise stimulate dopamine and endorphin release. These neurotransmitters (the chemical messengers in your brain) are crucial for motivation and mood regulation.
"Aerobic exercise activates reward pathways in the brain, effectively reducing cravings and relapse risk by restoring dopamine system function, which is often disrupted by chronic substance use." — National Institute on Drug Abuse1
In practice, movement-based interventions such as hiking, boxing, or team sports provide a natural route for the brain to relearn healthy pleasure responses. This is particularly relevant for men’s outdoor therapy, where challenging physical engagement aligns with the male brain’s responsiveness to action-oriented reward cues. Activity-based modalities have shown effect sizes comparable to some pharmacological treatments for mood and substance use disorders, suggesting these methods are far more than recreational—they are evidence-backed agents of neurobiological repair6.
Dopamine receptors can take 90 to 180 days to upregulate after chronic substance use. Movement-based therapies accelerate this healing by providing natural, healthy dopamine spikes. This bridges the critical gap during early sobriety when anhedonia (the inability to feel pleasure) is most severe.
This approach works best when individuals seek both physical engagement and measurable neurochemical impact as part of their recovery. Time investment varies, but most protocols recommend a minimum of 30–45 minutes of moderate to vigorous activity, three to five times per week, to achieve sustained benefits6.
With this foundation in brain chemistry, the next section explores how targeted cold exposure further enhances stress response and emotional resilience.
Readiness Assessment:

Cold exposure—such as ice baths or cold water immersion—offers a powerful tool for regulating the stress response system in men’s outdoor therapy. Technically, this process activates the parasympathetic nervous system (the network responsible for calming your body after a stressful event). Research has demonstrated that acute cold exposure can increase gamma-aminobutyric acid (GABA)—a neurotransmitter that dampens anxiety and promotes emotional stability—by as much as 40-50% in a single session5.
Over time, repeated exposure builds greater resilience to physical and psychological stress, supporting men who are navigating early sobriety when stress reactivity is often heightened. Consider this method if you are seeking to complement talk therapy with embodied, immediate nervous system regulation. Protocols typically recommend sessions of 2-5 minutes in water below 59°F (15°C), two to three times per week, but always under supervision for safety5. Ice bath setups range from low-cost DIY tubs (around $100) to commercial chillers ($1,000+), making it an accessible tool for many.
The following section will highlight why outdoor therapy uniquely resonates with men in structured recovery programs.
Decision Tool: Is Action-Oriented Therapy the Right Fit?
If you answered yes to two or more, action-based modalities may suit your recovery path.
For many men in recovery, traditional talk therapy can feel abstract or disconnected from daily life. Men's outdoor therapy fills this gap by introducing physically demanding alternatives—such as hiking, boxing, or ropes courses—that channel energy into direct engagement and skill-building. These experiences tap into the male brain’s preference for learning through doing, providing immediate feedback and a sense of tangible accomplishment.
Research reveals that men are 22% less likely to complete programs that rely heavily on talk therapy, but experience 18-25% higher engagement in activity-based models that include outdoor components8. At facilities like Trifecta Healthcare Institute, this movement-based programming is woven directly into the fabric of the recovery journey.
This path makes sense for professionals, veterans, or any man who finds motivation in physical challenge and visible progress. Sessions can require 1-2 hours per week for basic engagement, but more immersive programs may ask for several hours across consecutive days, especially in adventure-based formats. Resource needs typically include outdoor gear, trained facilitators, and access to natural spaces.
Up next: see how group-based challenges and accountability bring another dimension to men’s outdoor therapy.
Accountability Checklist: Maximizing Group-Based Recovery
If at least two points resonate, group-based outdoor therapy may be a strong fit.
Men’s outdoor therapy leverages group-based challenges—such as hiking expeditions, obstacle courses, or team sports—to cultivate accountability and authentic connection. Research indicates that men-only group programs encourage greater vulnerability disclosure and accountability-seeking behaviors, which are critical for sustained recovery9. The supportive dynamics of these settings help men confront setbacks openly, while peer-driven encouragement fosters resilience and adherence to sobriety goals.
In fact, adventure therapy participants experience 15–23% higher treatment completion rates and improved 12-month abstinence compared to those in conventional-only programs3. Opt for this framework when you are motivated by shared achievement and benefit from structured, brotherhood-oriented environments. Group-based outdoor sessions typically require access to trained facilitators, transportation to natural areas, and can range from weekly 2-hour outings to multi-day retreats, depending on program intensity.
Next, the discussion turns to how outdoor modalities integrate with clinical best practices to create multidimensional recovery pathways.
Integration Checklist: Are You Ready for Evidence-Based Adventure Therapy?
When these criteria are met, the stage is set for a multidimensional recovery experience.
When implemented alongside clinical best practices, men’s outdoor therapy creates a treatment dynamic that is both engaging and measurable. Adventure programming—such as guided hiking, ropes courses, or combat sports—serves as more than an energizing supplement. The physical and psychological challenges embedded in these activities reinforce lessons from cognitive behavioral therapy and trauma-informed care, making abstract skills like distress tolerance and emotional regulation actionable in real-world contexts.
| Treatment Component | Traditional Clinical Setting | Adventure-Integrated Therapy |
|---|---|---|
| Environment | Office or group room | Natural spaces, ropes courses, trails |
| Skill Application | Theoretical discussion | Real-time physical challenges |
| Peer Interaction | Verbal sharing | Shared physical obstacles and teamwork |
This strategy suits organizations that serve men who thrive on direct feedback, camaraderie, and accountability. Time and resource investment vary: immersive models may require several hours per week, specialized outdoor equipment, and facilitators trained in both evidence-based therapy and adventure programming. Such integration is particularly effective for professionals and veterans seeking structure, peer connection, and a sense of accomplishment beyond the therapy room.
By bridging clinical rigor with action-oriented modalities, this approach addresses core neurobiological and social drivers of addiction recovery for men3. Next, the focus shifts to trauma-informed outdoor interventions and their role in treating co-occurring conditions.
Decision Tool: Is Trauma-Informed Outdoor Intervention Warranted?
If any of these conditions apply, trauma-informed outdoor programming may offer a more integrated path to recovery.
Trauma-informed outdoor interventions combine principles of psychological safety with experiential activities in natural settings, specifically designed for men with co-occurring substance use and mental health conditions. It is important to note that facilities like Trifecta Healthcare Institute provide co-occurring mental health treatment alongside SUD support, rather than primary mental healthcare. These programs employ activities like guided wilderness expeditions, team-based adventure challenges, and mindfulness practices outdoors to gently activate and restore the nervous system’s stress response.
Research indicates that such interventions expand the "window of tolerance"—the range of emotional and physiological arousal a person can manage—thereby improving distress tolerance and reducing trauma-related relapse risk10. For men with trauma histories, the embodied experiences of movement, nature immersion, and peer support foster a sense of safety and control often missing in traditional therapy rooms.
This solution fits individuals who need to process trauma in a nonverbal, action-oriented format and benefit from somatic (body-based) healing mechanisms. Resource requirements typically include credentialed facilitators trained in both trauma-informed care and outdoor safety, access to wilderness areas, and supportive group structures. Sessions may span from weekly 2-3 hour outings to intensive multi-day adventures, depending on participant needs and treatment phase.
As men’s outdoor therapy increasingly integrates trauma-informed frameworks, the next section will outline practical steps for implementing these modalities in structured recovery journeys.
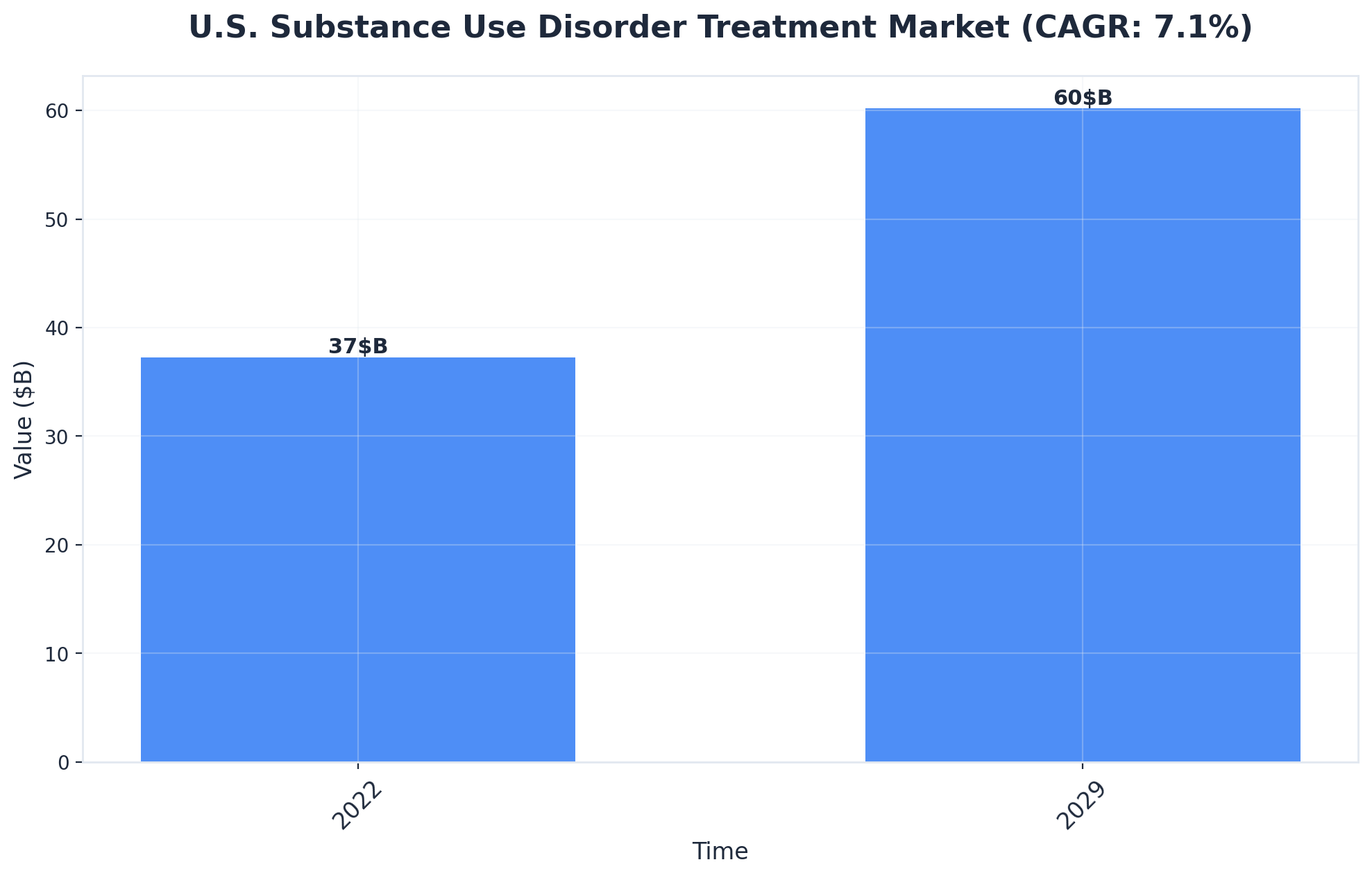
Outdoor adventure therapy functions most effectively when integrated into structured clinical programming rather than approached as a supplemental activity. The therapeutic value emerges not from nature exposure alone, but from how outdoor challenges interface with evidence-based treatment modalities within Partial Hospitalization Program (PHP) and Intensive Outpatient Program (IOP) frameworks. Facilities specializing in this integration—particularly a Nashville rehab or Knoxville rehab for men—demonstrate measurably stronger engagement and retention outcomes compared to traditional indoor-only approaches.
The clinical architecture matters significantly. Programs combining CBT and DBT with activities like ropes courses, white-water rafting, and technical hiking create environments where therapeutic concepts translate into embodied experience. During partial hospitalization programming, this structure proves particularly valuable: men apply distress tolerance skills while navigating challenging terrain, practice mindfulness during sustained physical exertion, and develop interpersonal effectiveness through team-based outdoor challenges.
// Sample Intensive Outpatient Program (IOP) Outdoor Integration 08:00 AM - Medical Check-in & Vitals 09:00 AM - Group CBT Session (Clinical) 10:30 AM - Outdoor Therapy: Ropes Course (Distress Tolerance) 12:30 PM - Lunch & Brotherhood Debrief 01:30 PM - Co-occurring Mental Health Support Group The Nashville rehab model pioneered by facilities like Trifecta demonstrates how outdoor adventure therapy functions as a delivery mechanism for evidence-based interventions, not merely as recreation. Program design determines therapeutic impact. Effective outdoor therapy within men's rehab settings incorporates intentional debriefing, connects physical challenges to recovery parallels, and builds progressively toward greater autonomy.
The brotherhood model—where men support each other through outdoor challenges while processing shared experiences—creates peer accountability structures that extend beyond clinical hours. For example, when facing a craving or frustration on the trail, men are taught to use the H A L T method (Hungry, Angry, Lonely, Tired) in real-time. Knoxville programs utilizing this approach report that men who engage deeply with outdoor components show stronger community integration and lower early dropout rates.
Dosage and progression protocols require careful calibration. Clinical outcomes improve when outdoor therapy sessions align with treatment intensity: more frequent integration during PHP phases, strategic placement within IOP schedules to maintain momentum, and transition planning that connects facility-based outdoor programming with community resources. Men's facilities in Tennessee increasingly structure outdoor activities as core treatment components rather than optional add-ons, recognizing that physical engagement often unlocks therapeutic progress where traditional talk therapy alone plateaus.
Year-round programming addresses a critical gap in treatment consistency. Facilities maintaining outdoor therapy through seasonal variations—winter hiking, cold-weather endurance challenges, adverse-condition training—report that men develop resilience skills directly transferable to recovery obstacles. The willingness to engage physically despite discomfort mirrors the psychological flexibility required for sustained sobriety. Nashville and Knoxville locations offering consistent outdoor programming regardless of weather demonstrate this commitment to therapeutic integrity over convenience.
The integration with alumni services and aftercare determines long-term effectiveness. Men transitioning from structured programming benefit when outdoor therapy continues through alumni activities, creating continuity between clinical treatment and independent recovery. Facilities offering ongoing outdoor adventure opportunities—group hikes, rafting trips, ropes course challenges—provide touchpoints that maintain brotherhood connections and therapeutic momentum.
This continuum approach, central to Trifecta's model, addresses the critical vulnerability period when men move from intensive treatment to community reintegration. Ultimately, outdoor therapy's clinical value lies in its capacity to bypass intellectual resistance and engage men through physical challenge and natural consequence. The most effective programs recognize this mechanism and structure outdoor components accordingly—not as amenities, but as therapeutic interventions with measurable treatment outcomes.
The outdoor therapy approaches that form the foundation of effective treatment must extend into long-term recovery to sustain healing. Sustainable sobriety requires more than completing a treatment program—it demands ongoing connection, purpose, and accountability that continues long after discharge. Men who build lasting recovery often credit the combination of peer support and physical engagement as essential protective factors against relapse.
According to research published in the Journal of Substance Abuse Treatment, individuals who maintain active peer support networks experience relapse rates 40-60% lower than those recovering in isolation. The brotherhood model at the core of a Nashville rehab and Knoxville rehab for men creates a network of men who understand the challenges of recovery firsthand, providing authentic support that extends beyond clinical settings into everyday life.
Movement-based activities serve as natural anchors for this community building, functioning as an extension of the outdoor therapy principles established during treatment. Training together in boxing or jiu-jitsu creates shared experiences that strengthen bonds while simultaneously addressing the physical and neurochemical aspects of healing discussed throughout this article. These activities provide structure, routine, and measurable progress—elements that support long-term recovery success.
At Trifecta's Nashville and Knoxville locations, the same activities that serve as therapeutic interventions during treatment become the foundation for alumni engagement, creating continuity between active treatment and lifelong recovery. Men who hiked together during PHP continue those trails in alumni outings; those who trained in boxing during IOP maintain those partnerships in ongoing sessions.
Research from the American Journal of Drug and Alcohol Abuse demonstrates that men in recovery who maintain regular physical activity experience relapse rates 50% lower than sedentary peers, while those with strong peer connections show similarly reduced rates. The integration of movement with brotherhood support addresses both the physiological need for healthy dopamine regulation and the psychological need for belonging.
This dual approach helps men develop sustainable coping mechanisms while building a recovery community that continues supporting them long after formal treatment ends. Trifecta's alumni services and aftercare programming maintain this integrated model, offering ongoing access to movement-based activities and brotherhood support that extend the therapeutic benefits of outdoor therapy into sustained, long-term sobriety. The men's rehab model proves most effective when treatment philosophy becomes lifestyle philosophy—when the outdoor therapy that initiates healing becomes the community practice that sustains it.
Choosing between outdoor-integrated programs and conventional treatment depends on the individual’s clinical needs, recovery goals, and engagement style. Outdoor-integrated models—such as men’s outdoor therapy—work well for those motivated by physical activity, group accountability, and experiential learning. Research shows men are 18–25% more engaged in activity-based programs and complete treatment at higher rates compared to talk-therapy-intensive models 8. Conventional approaches may be necessary during acute withdrawal or when medical stabilization and close psychiatric oversight are required. This approach is ideal for men seeking a blend of evidence-based therapy with action-oriented recovery. Consult with a clinical provider to determine the best fit for your stage of recovery.
For measurable neurochemical benefits in men’s outdoor therapy, research indicates a protocol of 30–45 minutes of moderate to vigorous physical activity, three to five times per week, is optimal. Activities such as hiking, boxing, or team sports reliably stimulate dopamine and endorphin release, both of which are critical for restoring reward pathways disrupted by substance use 6. Cold exposure—like ice baths—can also be effective when practiced two to three times weekly for 2–5 minutes per session, supporting GABA increases and stress regulation 5. This level of intensity and frequency aligns with outcomes seen in evidence-based recovery programs for men.
Outdoor therapy—including movement-based and nature-focused modalities—should not serve as the sole or primary treatment during acute withdrawal phases. Acute withdrawal, also called detoxification, is a medically complex period that can involve severe symptoms requiring close monitoring, medication, and clinical stabilization. While men’s outdoor therapy can play a supportive role in the broader recovery process, leading addiction medicine organizations recommend evidence-based medical detox and psychiatric oversight during the initial withdrawal period before introducing physical or adventure-based activities 2. This approach works best when outdoor therapy is sequenced after medical stabilization, ensuring safety and optimizing long-term engagement.
Most men engaging in movement-based programming begin to notice mood stabilization, reduced cravings, and increased energy within the first few weeks, especially when following protocols of 30–45 minutes of moderate to vigorous activity three to five times per week 6. However, research shows that sustained recovery outcomes—such as higher treatment completion and maintained abstinence—typically emerge after three to six months of consistent participation in men’s outdoor therapy 3. This timeframe reflects the period needed for neurochemical and behavioral changes to consolidate. Peer accountability and group involvement can accelerate these benefits, making this approach well-suited for those seeking durable transformation through active, community-driven recovery.
Men-only outdoor programming is often more effective than mixed-gender approaches due to increased vulnerability, accountability, and peer bonding specific to male recovery pathways. Research indicates that men in gender-specific groups are more likely to disclose struggles, seek accountability, and support each other in ways that directly promote sustained engagement and abstinence 9. These environments foster a sense of brotherhood and shared challenge, which can be especially impactful for men who might otherwise hesitate to open up in mixed company. This approach is ideal for professionals and veterans who value camaraderie, direct feedback, and authentic connection as part of their recovery journey through men’s outdoor therapy.
Yes, outdoor therapy programs are available across a range of budget levels in Tennessee. Options include low-cost community-based activities, nonprofit-supported initiatives, and more intensive private programs that integrate clinical supports with adventure-based modalities. Accessibility often depends on factors like facilitator expertise, program length, and the inclusion of specialized activities or evidence-based therapies. While research highlights the effectiveness of men’s outdoor therapy in various formats, it also notes that resource requirements—such as gear, transportation, and facilitator training—can impact affordability and access, particularly in rural versus urban settings 2. Prospective participants are encouraged to explore local program offerings and financial assistance options to find a suitable fit.


April 13, 2026

April 15, 2026

April 15, 2026