
April 13, 2026
Learn how alumni services support men with co-occurring trauma through engagement, therapy, and relapse prevention with Trifecta Healthcare Institute.
Start Your Journey NowWritten and reviewed by the clinical team at Trifecta Healthcare Institute, a men’s-only treatment center in Tennessee specializing in substance use, mental health, and dual diagnosis care.
Neurobiological recovery extends far beyond the completion of detoxification or even primary residential treatment. For professionals designing alumni services for man with co-occurring trauma, understanding that the brain’s stress and reward circuits remain in flux long after physical withdrawal symptoms subside is critical. Research shows that individuals with complex trauma and substance use disorders (SUD) often experience enduring challenges with executive function, impulse control, and emotional regulation—areas governed by brain systems that require sustained intervention and support.7
Alumni programming plays a vital role in addressing these ongoing neurobiological needs. Structured movement-based programming, peer accountability, and trauma-informed alumni activities have demonstrated greater effectiveness in supporting brain recovery than traditional talk therapy alone. This is especially true for men who respond well to action-oriented modalities and the brotherhood found in a dedicated men's drug rehab environment.7
This approach is ideal for facilities that include regular opportunities for physical activity, ongoing peer connection, and trauma-sensitive check-ins to reinforce new neural pathways. Prioritizing these elements can help mitigate the risk of relapse tied to persistent neurobiological vulnerabilities. Understanding these brain-based challenges sets the stage for examining why the first six months post-discharge represent a uniquely high-risk period for relapse.
Checklist: Risk Factors During the 0-6 Month Window
The initial six months following treatment discharge mark the period of greatest vulnerability for a man with co-occurring trauma and substance use disorder. Neurobiological instability, loss of structured support, and unaddressed trauma triggers converge to elevate relapse and overdose risk. Data shows men account for roughly 70% of overdose deaths, with mortality risk peaking in this early post-discharge phase—a risk that drops by 40% when consistent alumni engagement is present.6
Alumni services counteract this window of risk by maintaining connection, structure, and trauma-informed support when the protective environment of treatment is no longer present. This solution fits organizations navigating major life transitions for their clients, such as returning to high-stress workplaces or environments without established sober networks. Opt for alumni frameworks that emphasize immediate post-discharge outreach, frequent check-ins, and rapid access to movement-based or peer-led resources.
Prioritizing robust alumni connection during this period can be decisive in interrupting the relapse cycle. Next, a closer look at integrated alumni frameworks reveals how trauma and SUD support can be woven together for lasting stability.

Checklist: Core Elements of Recovery Management Checkup Protocols
Recovery management checkups (RMCs) are structured, periodic assessments designed to identify early warning signs of relapse and re-engage men with co-occurring trauma and substance use disorders before setbacks escalate. Unlike reactive crisis intervention, RMCs operate as proactive touchpoints—typically every one to three months—where alumni connect with trained staff or peer specialists for brief check-ins, symptom monitoring, and barrier identification. Trifecta Healthcare Institute utilizes this model to ensure co-occurring mental health treatment alongside SUD support remains consistent.
"Quarterly recovery management checkups operate as proactive touchpoints, reducing substance use relapse episodes by 25-40% and sustaining engagement for 18 months or longer."
Evidence demonstrates that individuals receiving quarterly RMCs experience a significant reduction in substance use relapse episodes and maintain engagement with support systems long after primary treatment. RMCs are most effective when they incorporate trauma-informed screening, support for executive function challenges, and immediate referral pathways to peer or movement-based programming if symptoms escalate.4
Consider this method if your alumni population includes men at high risk for disengagement, those navigating complex trauma histories, or individuals returning to environments with minimal external support. Embedding RMCs into the alumni framework provides a safety net that can substantially extend recovery stability. Next, the discussion turns to the architecture of peer support specifically tailored for men, examining how brotherhood-based models can further reinforce long-term engagement.
Checklist: Hallmarks of Effective Male Peer Support Architecture
Peer support architecture for men with co-occurring trauma must move beyond generic support group models, instead prioritizing brotherhood, shared experience, and actionable engagement. Research indicates peer-led alumni groups tailored for men maintain sustained engagement rates of 45–60%, significantly higher than the 20–30% seen in purely clinician-led models. This strategy suits organizations that serve men reluctant to participate in traditional talk therapy or who seek camaraderie rooted in mutual challenge and support.5
Comparison of Alumni Support Architectures
A robust peer framework typically includes trauma-informed facilitators—often men in long-term recovery who can model vulnerability and resilience. These groups emphasize mutual accountability, problem-solving, and movement-based or outdoor activities that foster genuine bonds. The integration of confidentiality, respect, and structured check-ins supports a psychologically safe environment, which is crucial for men navigating shame or stigma tied to trauma and substance use.
Peer support models benefit from flexible formats, offering both in-person and virtual participation to accommodate alumni with demanding schedules or those who relocate. Consider this route if your alumni services must balance autonomy with collective accountability and appeal to men who thrive on action, brotherhood, and shared purpose. Moving forward, the role of movement-based programming will be explored, revealing how physical activity acts as a neurobiological tool in sustaining recovery.
Checklist: Elements of Effective Activity Therapy in Alumni Services
Activity therapy refers to the intentional use of physical movement and experiential challenges as a core component of alumni programming for men with co-occurring trauma and substance use disorder. Neurobiologically, this approach targets the same brain circuits—such as the prefrontal cortex and limbic system—that are implicated in both trauma-related dysregulation and addictive behavior. Research highlights that structured activity-based interventions outperform talk therapy alone in improving executive function, impulse control, and emotional stability among this population.7
This method works when alumni services intentionally weave activities like martial arts, adventure outings, or cold exposure into ongoing recovery support. For example, boxing and jiu-jitsu offer a dual benefit: regulating stress hormones while promoting peer connection and accountability. Trauma-informed facilitation ensures safety and scalability, allowing men to participate regardless of physical ability.
Activity therapy is ideal for alumni populations where traditional verbal processing falls short, or where sustained engagement hinges on action and camaraderie. By providing a neurobiological reset and fostering resilience, these movement-based models help break the cycle of relapse and emotional shutdown. The next section will explore how brotherhood accountability structures further reinforce these gains and promote long-term stability.
Checklist: Core Components of Brotherhood Accountability Structures
Brotherhood accountability structures are designed to meet the unique relational and motivational needs of men with co-occurring trauma and substance use disorders. Unlike top-down monitoring, these frameworks build a culture where commitment is to the group as much as to oneself. Peer-led cohorts, often modeled after therapeutic communities, assign leadership responsibilities and foster a sense of belonging through shared challenge, open disclosure, and mutual encouragement.
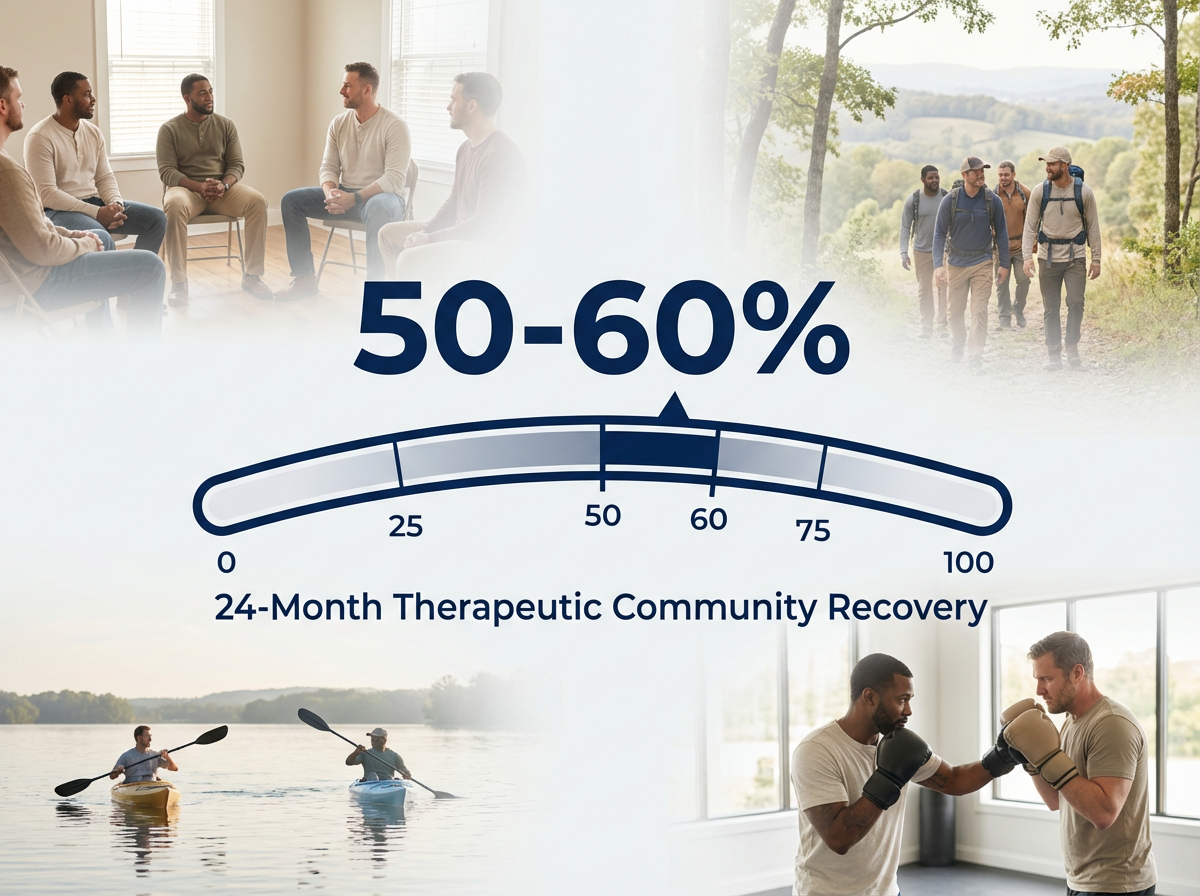
Research shows that alumni services integrating structured peer accountability, such as in therapeutic community models, achieve sustained recovery rates of 50–60% at two years—substantially higher than unstructured or clinician-only models. Importantly, these structures are most effective when alumni are empowered to set personal and group recovery goals and are encouraged to take on mentorship roles as their stability grows. This approach works best when trauma-informed practices are embedded, reducing re-traumatization by 60–70% and strengthening long-term engagement.8,10
Prioritize brotherhood accountability when fostering a culture of mutual responsibility, especially for alumni who thrive on collective action and peer-driven support. The following section will illustrate how this sense of brotherhood and accountability extends to practical domains like housing, employment, and daily stability.
Checklist: Key Stability Metrics for Alumni with Co-occurring Trauma
For a man with co-occurring trauma, stability in housing and employment is both a measure and a driver of long-term recovery. Alumni services that integrate practical life domain support—such as assistance with sober living placement, job readiness coaching, and daily routine planning—demonstrate up to 50% improvement in 12-month housing stability for participants, especially veterans and those with high trauma exposure.3
These outcomes hinge on a coordinated approach: trauma-informed peer mentoring, proactive check-ins, and rapid linkage to local resources. This path makes sense for alumni populations facing unstable living conditions, employment gaps, or who lack robust social networks. Prioritize alumni programming that not only tracks these life metrics but actively intervenes when setbacks occur. Close monitoring enables rapid response to housing loss or job changes, which are common relapse triggers for men with layered trauma histories.
Checklist: Core Metrics for Sustained Recovery Success in Alumni Services
Measuring the impact of alumni services requires a multidimensional approach. Key indicators include reduced relapse rates over 12–24 months, which are typically 30–40% lower among those engaged in structured alumni programming compared to those without ongoing support. Peer-led groups and trauma-informed check-in protocols show a sustained engagement rate of 45–60% after primary treatment, highlighting the effectiveness of integrated models.2,5
When tracking these metrics in your facility's CRM, you might use custom data payloads to ensure accurate reporting. For example:
To quickly save these records during a live check-in, use Ctrl + S or your system's equivalent shortcut. Tracking metrics such as housing and employment stability, frequency of alumni participation, and decreases in trauma-related setbacks provides actionable data for continuous improvement.
Prioritize this when alumni data is collected at regular intervals, using both quantitative (participation, relapse, employment) and qualitative (self-reported well-being, peer feedback) measures. Frameworks that allow for rapid response to challenges, and consider alumni progression to peer or leadership roles, serve as a strong marker of long-term recovery success.
Checklist: What to Look for in Trauma-Integrated Alumni Programming
Effective alumni engagement for men with co-occurring trauma goes beyond scheduled check-ins—it requires a living, breathing brotherhood that moves with you through the ongoing work of recovery. The research is clear: alumni programming works best when it combines proactive peer connection, structured support, action-based activities, and real-world stability resources, all within a trauma-informed framework.2,5
As you evaluate alumni options after treatment—whether you completed programming at a Nashville rehab, Knoxville facility, or elsewhere—look for communities that understand male relational dynamics and offer more than talk. The most effective programs integrate movement (think boxing sessions, hiking groups, or jiu-jitsu training) with consistent peer accountability, creating the kind of brotherhood that sustains recovery when motivation alone isn't enough. Consider this route if you are seeking long-term stability, reduced relapse risk, and genuine connection beyond the treatment center walls.
Once you're connected to alumni programming that addresses both your trauma history and substance use recovery, ongoing participation and honest engagement ensure the support continues delivering meaningful results in your daily life.
When you or someone you love are ready to begin healing—mind, body, and spirit—connect with Trifecta Healthcare Institute. We help men thrive in and out of treatment.
Peer-led programming for alumni services for man with co-occurring trauma offers distinct advantages: higher sustained engagement (45–60% vs. 20–30% in clinician-only models), stronger peer accountability, and relatable mentorship—key for men who value autonomy and brotherhood. This approach is ideal when participants respond best to shared experience and action-based support. In contrast, clinician-led programs provide structured oversight, greater clinical expertise, and may be preferable for men with severe psychiatric needs or those early in trauma recovery. Consider peer-led models when fostering camaraderie and long-term engagement, and clinician-led if clinical complexity or stabilization is a priority.5
Comprehensive alumni services for a man with co-occurring trauma—including trauma-informed peer engagement, structured activity-based programming, and ongoing recovery management checkups—require significant resources, but exact cost ranges are rarely published publicly. While many peer-led models demonstrate 35–40% cost savings compared to clinician-only frameworks, total costs vary based on service intensity, frequency of contact, and integration of housing or vocational supports. Organizations should anticipate higher investment for programs that embed both trauma and substance use disorder (SUD) support with robust alumni infrastructure. This approach works best when combined with outcome tracking to ensure resource allocation matches measurable recovery gains.9
Most organizations observe initial measurable outcomes from structured alumni engagement protocols for men with co-occurring trauma within the first 3 to 6 months. Key metrics—such as reduced relapse rates, increased peer participation, and improved daily stability—typically begin to emerge in this window, with research showing that quarterly recovery management checkups alone can reduce relapse episodes by 25–40% and extend engagement beyond 18 months. This approach works best when alumni services for man with co-occurring trauma include proactive outreach and trauma-informed programming, as positive trends often strengthen over the first year with consistent engagement.4
For alumni services for man with co-occurring trauma, the most effective frequency for recovery management checkups during the first year post-treatment is quarterly—every three months. Research shows this schedule reduces relapse episodes by 25–40% and helps sustain engagement for 18 months or longer after discharge. Monthly checkups may be warranted for individuals with high relapse risk or minimal external support, but quarterly remains the evidence-based standard for most. This approach works best when each checkup includes trauma-informed screening and rapid referral pathways to peer or movement-based programming if needed.4
Alumni services for man with co-occurring trauma can address persistent executive function deficits—such as challenges with focus, planning, and impulse control—through structured activity-based programming, trauma-informed peer accountability, and regular recovery management checkups. Research shows these approaches target neurobiological pathways linked to executive dysfunction and outperform traditional talk therapy alone in this population. This path makes sense for alumni who continue to struggle with organization, decision-making, or emotional regulation after primary treatment. Integrating movement-based activities and peer-led support helps reinforce daily routines, strengthen cognitive skills, and reduce relapse risk tied to executive function challenges.7
For remote alumni engagement, platforms that prioritize video-based group meetings (like Zoom or Microsoft Teams) and secure, private community apps (such as Slack or Circle) best replicate the authenticity of in-person peer connection. These tools allow trauma-informed, action-oriented alumni services for man with co-occurring trauma to maintain brotherhood, accountability, and real-time interaction even at a distance. Research indicates hybrid models—combining scheduled video check-ins with asynchronous group chats—achieve sustained engagement rates of 45–60%, outperforming text-only or purely automated solutions. Opt for platforms that offer both privacy controls and options for movement-based or challenge-oriented virtual events, as these features reinforce trust and belonging in a men’s recovery community.5
Tennessee-specific alumni programs reflect notable regional differences between Nashville and Knoxville. Nashville alumni services for man with co-occurring trauma often emphasize integration with a larger, more diverse recovery community and feature expanded access to structured movement-based activities like boxing and outdoor adventure, leveraging the city’s urban resources. In contrast, Knoxville programs may prioritize smaller cohort sizes, greater peer intimacy, and frequent outdoor engagement—such as hiking or ropes courses—taking advantage of the surrounding natural environment. Both regions maintain a strong focus on trauma-informed, brotherhood-driven support, but the blend of activities and community partnerships may be tailored to local culture and resources. This method works when alumni services remain flexible and regionally responsive, ensuring men with co-occurring trauma access programming that resonates with their lived experience and recovery environment.5


April 13, 2026

April 15, 2026

April 15, 2026