
April 13, 2026
Explore how boxing therapy Tennessee programs combine trauma-informed care and movement to support recovery in major cities at Trifecta Healthcare Institute.
Start Your Journey NowWritten and reviewed by the clinical team at Trifecta Healthcare Institute, a men’s-only treatment center in Tennessee specializing in substance use, mental health, and dual diagnosis care.
As Tennessee introduces new legislative frameworks supporting holistic addiction treatment, boxing therapy Tennessee is rapidly gaining traction among clinical professionals and active men seeking dynamic recovery solutions. Emerging neuroscience reveals exactly why this approach works for professionals who find traditional talk therapy insufficient. High-intensity boxing activates the parasympathetic nervous system, generating neurochemical changes that down-regulate the amygdala—a core region involved in trauma and stress responses—and support emotional rebalancing.1
Studies show that within four to six weeks, consistent engagement in combat sports like boxing increases vagal tone and boosts production of brain-derived neurotrophic factor (BDNF), which is vital for neuroplasticity and executive function. These neurobiological adaptations translate to improved emotional regulation, impulse control, and resilience—critical outcomes for men navigating substance use and co-occurring mental health conditions in Tennessee’s high-stress environments.1
"Combat-based therapies facilitate therapeutic exposure by simultaneously engaging threat-detection systems and higher-order thinking, creating a unique context for trauma processing unavailable in sedentary interventions."7
As Tennessee’s health systems—particularly in metro hubs such as Nashville and Knoxville—integrate movement-based models, the region is poised to set new standards for active recovery grounded in neuroscience. Building on these neurobiological foundations, we must examine how Tennessee’s geography and cultural attitudes shape the delivery of movement therapy statewide.9
Tennessee’s varied geography—from the rugged trails of the Smoky Mountains to the greenways threading through Nashville and Knoxville—naturally lends itself to movement-based recovery approaches. For men seeking a hands-on path to healing, movement therapy has found fertile ground across the state, with program offerings expanding in both metro and rural regions. State health data confirms that demand for movement therapy is rising; the 2025 Tennessee health assessment reported a significant uptick in male enrollment for active recovery programs, particularly in areas where traditional talk therapy underperforms for engagement and retention.9
Local cultural values also shape how these therapies are embraced. Tennessee’s strong tradition of athletics, outdoor adventure, and male camaraderie aligns perfectly with the active, brotherhood-oriented elements of movement therapy. This alignment is especially evident in places like the Nashville metro and Knoxville’s foothills, where programs integrate boxing sessions with group outdoor activities and peer support groups. Regulatory guidance now recognizes movement-based modalities as evidence-based complements to standard care, provided they are delivered with robust clinical oversight.2
Movement-based programs have demonstrated substantial benefits for emotional regulation and post-traumatic stress outcomes, especially among men navigating trauma histories or chronic stress. Controlled studies show that individuals participating in boxing-based interventions experience 31–47% greater improvements in emotional regulation and hypervigilance reduction compared to those receiving only traditional talk therapy. This effect is particularly relevant in Tennessee’s high-stress metro environments like Nashville and Knoxville, where professional men often face unique occupational and familial pressures.4
The therapeutic value of boxing lies in its ability to activate both the body’s threat-detection systems and the executive function centers of the brain. By requiring simultaneous engagement of the amygdala and prefrontal cortex, boxing therapy creates a safe, embodied platform for trauma processing. Key clinical benefits include:7
Updated guidelines from the American Psychological Association now recognize combat-based movement therapies as evidence-supported complements to standard trauma treatment, provided they are delivered with clinical oversight. As Tennessee’s treatment centers adopt these models, they are witnessing measurable reductions in PTSD symptoms and improved emotional stability among participants.2
Addiction recovery programs throughout Tennessee have increasingly adopted movement-based interventions as a strategic response to the state’s historically low SUD treatment capacity and high relapse rates. These models, particularly in metro areas like Nashville and Knoxville, provide an active structure that addresses both the neurochemical imbalances and behavioral triggers associated with substance use disorders.9
Figure 1: Conceptual representation of relapse risk reduction when integrating high-intensity physical activity into standard SUD treatment protocols.
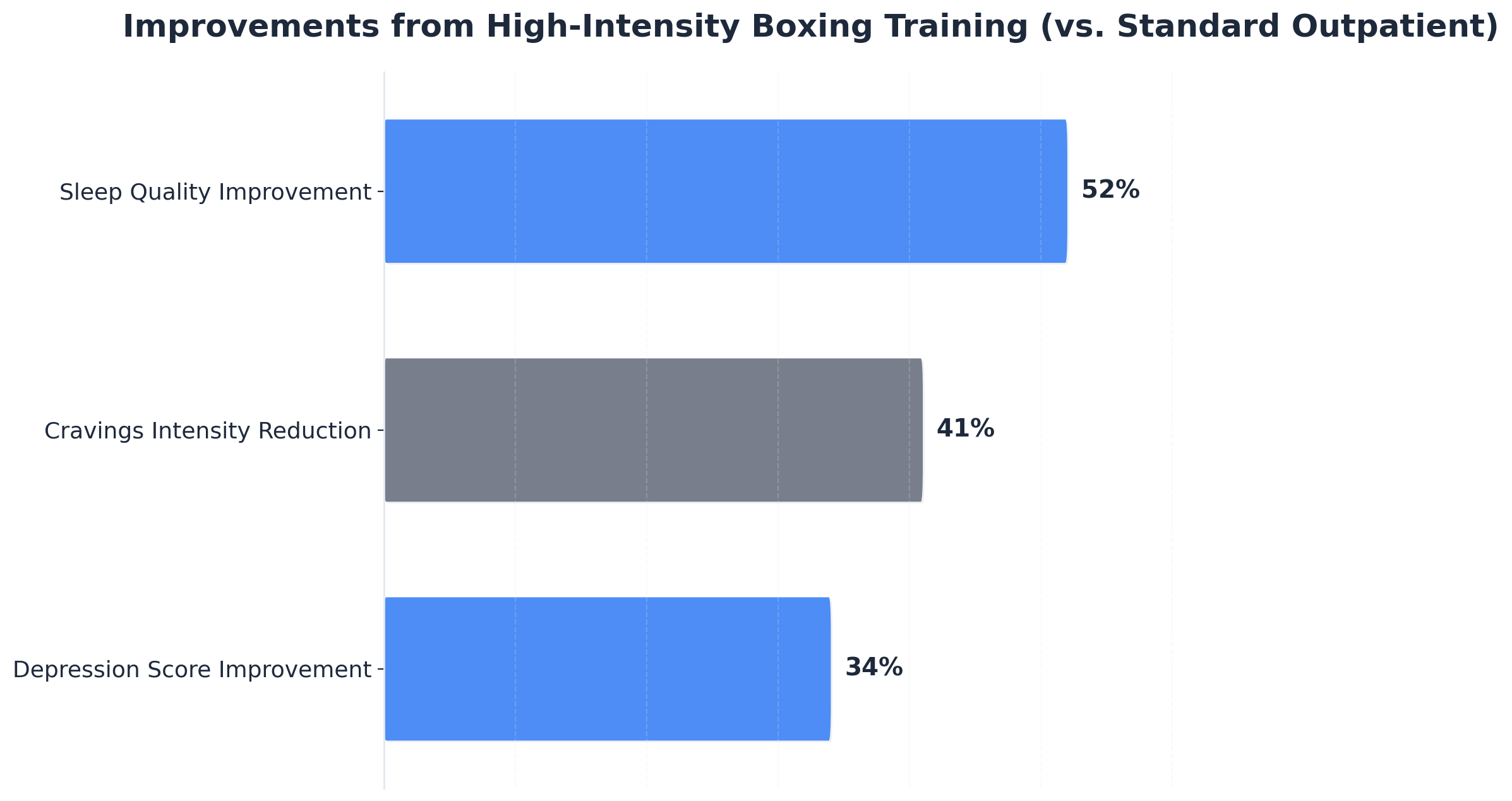
Recent clinical studies report that men participating in high-intensity boxing interventions demonstrate a 41% reduction in cravings and a 52% improvement in sleep quality compared to those enrolled in standard outpatient programs. These effects play a pivotal role in relapse prevention, as disrupted sleep and unmanaged cravings are leading predictors of early return to use. Boxing’s demand for focus and physical exertion also serves as an immediate coping mechanism, channeling stress and agitation into purposeful movement rather than substance-seeking behaviors.6,7
Tennessee-specific data highlights the practical impact of these programs: regions that have integrated structured combat sports into dual diagnosis care, such as Davidson and Knox counties, report improved long-term retention and fewer relapse-related emergency visits. By emphasizing accountability and peer support within the boxing context, these initiatives align with the state’s cultural values of camaraderie and resilience.9
Regional disparities continue to shape the availability of specialized programs for men seeking movement-based recovery. State health data from 2025 confirm that Tennessee’s substance use disorder treatment capacity remains 34% below the national average, with the most pronounced gaps occurring outside major hubs like Nashville and Knoxville. In regions such as the Tri-Cities, the Upper Cumberland, and the West Tennessee Delta, limited clinical infrastructure and a shortage of trained staff make it challenging to deliver evidence-based boxing interventions.9
These service gaps are especially acute for working-age men in rural areas who prefer active engagement over traditional talk therapy, reinforcing existing barriers to long-term recovery. While some metro areas are expanding their offerings, rural and underserved communities still face waitlists or must travel considerable distances to participate in structured movement therapy. State regulators have begun to address these inequities by supporting telehealth consults and incentivizing training for movement-based clinicians, but access remains uneven.9
Nashville and Knoxville have emerged as leading centers for movement-based recovery, establishing models that blend clinical rigor with deep local engagement. In a typical Nashville rehab setting, program structures integrate boxing and movement-based therapy into partial hospitalization and intensive outpatient frameworks, ensuring robust clinical oversight and strong coordination with co-occurring mental health care. These programs often link boxing sessions with group therapy, trauma-informed counseling, and peer accountability—tailoring intervention intensity to the needs of professional men and veterans in the city’s fast-paced, high-stress landscape.2
A Knoxville rehab for men draws on the region’s culture of outdoor adventure and athletic brotherhood, weaving boxing therapy into broader movement programming that includes hiking, ropes courses, and team-based physical challenges. The foothills setting allows for creative integration of outdoor elements, fostering resilience and camaraderie among participants. Across both metros, the inclusion of these therapies aligns with the state’s regulatory guidance for evidence-based, male-specific care, and has driven measurable improvements in engagement and retention compared to standard outpatient models.9
Movement-based recovery represents more than an alternative therapeutic approach—it addresses a fundamental gap in traditional addiction treatment for men who've spent years disconnected from their bodies, their instincts, and their capacity for physical engagement with the world. When substance use disorders take hold, they don't just hijack neurochemistry; they sever the relationship between mind and body, leaving men navigating recovery through talk therapy alone, often without the physical outlet that makes emotional processing sustainable.
Boxing, jiu-jitsu, hiking, and structured physical challenges create neurobiological changes that support recovery: they regulate stress response systems, restore dopamine function, and rebuild the mind-body connection that addiction fractures. For programs integrating these methodologies into evidence-based treatment frameworks, the challenge becomes maintaining therapeutic integrity while innovating beyond conventional approaches. This requires navigating the same regulatory landscape that governs all addiction treatment—but with intentional documentation that demonstrates how movement-based interventions achieve clinical outcomes.
As industry peers, you understand that the oversight mechanisms governing addiction treatment in Tennessee establish the foundation that allows innovative programming to flourish with accountability. Quality facilities maintain rigorous implementation standards through multiple oversight mechanisms. Accreditation bodies such as The Joint Commission and the Commission on Accreditation of Rehabilitation Facilities (CARF) establish baseline requirements for clinical operations, staff qualifications, and patient safety protocols. When navigating state compliance databases, using Ctrl + F to search for specific movement-therapy mandates reveals that these organizations conduct regular audits to ensure facilities maintain evidence-based practices and ethical treatment standards.
State licensing boards provide additional regulatory oversight specific to Tennessee's healthcare requirements. The Tennessee Department of Mental Health and Substance Abuse Services monitors compliance with state regulations, including staff-to-patient ratios, documentation standards, and facility safety measures. Documenting these interventions often requires specific ICD-10 and CPT codes to ensure compliance. Licensed facilities must demonstrate adherence to both clinical and operational benchmarks to maintain their credentials.
Professional treatment centers implement internal quality assurance programs that extend beyond minimum regulatory requirements. Clinical supervisors conduct regular case reviews, treatment teams evaluate patient progress through standardized assessments, and peer consultation ensures therapeutic interventions align with current research. These internal mechanisms create accountability structures that support consistent, high-quality care delivery.
For men's Nashville rehab and Knoxville rehab programs that integrate boxing therapy, outdoor adventure activities, and other movement-based interventions, this regulatory framework becomes the structure that validates innovation. Facilities embracing comprehensive accreditation demonstrate that non-traditional therapeutic approaches aren't alternatives to evidence-based care—they're enhancements that meet the same rigorous standards while addressing the physical dimension of recovery that conventional treatment often overlooks.
The intersection of regulatory compliance and innovative treatment methodologies requires careful documentation and outcome tracking. Programs incorporating movement-based therapies, trauma-informed care, and co-occurring mental health support must demonstrate clinical efficacy through data collection and peer-reviewed protocols. This dual focus on innovation and accountability ensures that evolving treatment approaches maintain therapeutic integrity while meeting established healthcare standards—creating pathways for men who need recovery programs that engage both body and mind, not just one or the other.

Quality standards and regulatory frameworks create the foundation that enables innovative, specialized approaches to treatment—including the gender-specific programming that many men find essential to their recovery. Men-only programming creates unique therapeutic advantages that mixed-gender environments often cannot replicate. When you engage in recovery alongside other men facing similar challenges, you develop accountability structures rooted in shared experience rather than performance or image management. This dynamic proves particularly valuable if you've historically struggled to express vulnerability or acknowledge emotional needs in traditional therapeutic settings.
The brotherhood model extends beyond simple peer support. Many of us carry internalized expectations about strength, self-sufficiency, and emotional control that can obstruct healing. Male-specific programming addresses these barriers directly, creating space where you can explore trauma, shame, and fear without the social dynamics that frequently inhibit honest communication. At Trifecta Healthcare Institute's Nashville and Knoxville locations, this brotherhood philosophy operates through structured daily interactions—from group therapy sessions where men hold each other accountable to shared physical training that builds trust through action rather than words alone. The sober living environments reinforce this foundation of mutual support and authentic connection, creating a recovery community that extends beyond clinical hours.
Movement-based activities amplify these benefits by shifting therapeutic engagement from purely cognitive processing to embodied experience. Boxing sessions, jiu-jitsu training, and outdoor challenges provide natural contexts for building trust, practicing healthy competition, and developing resilience through shared physical effort. These activities create opportunities to support one another through difficulty, celebrate progress, and establish bonds that extend beyond treatment completion.
The neurochemical benefits of physical activity combine with the psychological safety of male-specific environments to accelerate healing. Men who might resist traditional talk therapy often engage more readily when therapeutic work occurs alongside tangible physical challenges. This approach proves especially effective for professionals, veterans, and men seeking alternatives to conventional treatment models. The result is a recovery experience that honors masculine identity while dismantling the isolation that substance use disorders create.
The brotherhood dynamic that emerges through male-specific programming creates the foundation for truly integrated care—when men develop trust and accountability through shared physical challenges, they become more receptive to the full spectrum of therapeutic interventions. Boxing therapy doesn't exist in isolation—it functions as one component within a comprehensive treatment framework. At facilities offering movement-based programming, boxing sessions complement evidence-based modalities like CBT, DBT, and EMDR to address the full spectrum of substance use disorders and co-occurring mental health conditions. It is important to note that Trifecta focuses on co-occurring mental health treatment alongside SUD support, rather than primary mental healthcare.
This integrated approach recognizes that men in recovery benefit from multiple therapeutic touchpoints throughout their day. A morning boxing session might precede individual therapy, where the emotional release from physical exertion creates openings for deeper psychological work. Group therapy sessions can process insights gained during movement activities, while trauma-focused treatments address underlying issues that boxing alone cannot resolve.
The continuum of care ensures boxing remains accessible as men progress through recovery stages:
Consider a typical recovery trajectory at a Nashville rehab for men: a participant enters medical detox experiencing acute withdrawal symptoms and emotional dysregulation. Within days, as medical stabilization occurs, he begins attending supervised boxing sessions in the partial hospitalization program—initially just learning basic movements and breathing techniques. By week three, he's incorporating boxing into his morning routine before individual CBT sessions, where his therapist notices he's processing anger and shame more effectively.
Transitioning to intensive outpatient programming, he maintains boxing three times weekly while returning to work, using the structured physical outlet to manage workplace stress without relapse. Six months post-treatment, he continues attending alumni boxing sessions, where the same brotherhood that supported his early recovery now reinforces his long-term wellness practices.
This integration matters because recovery outcomes depend not on any single intervention, but on creating sustainable lifestyle patterns that address biological, psychological, and social dimensions simultaneously. Research consistently demonstrates that individuals who maintain regular physical activity during recovery show significantly lower relapse rates—some studies indicating up to 40% reduction in substance use recurrence. When boxing becomes woven into the fabric of comprehensive care rather than treated as an isolated amenity, it transforms from a temporary coping mechanism into a permanent pillar of sustained recovery, providing men with both immediate neurochemical regulation and long-term resilience against the triggers and stressors that threaten sobriety.
Boxing therapy represents more than an innovative treatment modality—it embodies a fundamental shift in how men approach recovery from substance use disorders and co-occurring mental health conditions. The integration of structured physical training with evidence-based therapies like CBT, DBT, and trauma-informed care creates a comprehensive framework that addresses addiction's neurological, psychological, and social dimensions simultaneously.
The model's effectiveness stems from the convergence of three critical elements: regulatory oversight that enables innovative approaches while maintaining clinical rigor, male-specific programming that leverages competitive drive and peer accountability, and neuroscience-backed movement protocols that restore neurochemical balance disrupted by substance use. For men seeking alternatives to traditional talk therapy approaches, this combination offers tangible progress markers and immediate feedback that reinforce commitment to recovery.
Programs like those offered at Trifecta Healthcare Institute's Nashville and Knoxville locations demonstrate how boxing can integrate seamlessly into a broader continuum including medical detox, PHP, IOP, and structured sober living. When physical discipline becomes part of comprehensive care rather than an isolated activity, men gain access to tools that serve them long after formal treatment concludes. The brotherhood forged through shared physical challenges creates accountability networks that support long-term healing and community reintegration. For men across Tennessee navigating the complexities of addiction recovery, movement-based programming represents not simply an alternative approach, but a paradigm shift that aligns treatment with how men naturally process challenge, build resilience, and sustain lasting change.
When you or someone you love are ready to begin healing—mind, body, and spirit—connect with Trifecta Healthcare Institute. We help men thrive in and out of treatment.
Clinicians delivering boxing therapy Tennessee must hold a valid Tennessee mental health license—such as LPC, LCSW, LMFT, or psychologist credentials—and possess specialized training in trauma-informed care or substance use disorder treatment. State regulations require that all combat-based interventions be supervised by these licensed professionals, who must also demonstrate competency in risk assessment and de-escalation protocols. The Department of Mental Health & Substance Abuse Services further mandates ongoing professional development and formal intake procedures to ensure participant safety, especially for men with complex trauma backgrounds. Peer facilitators may support sessions, but only under direct clinical oversight.2,9
Boxing therapy Tennessee programs are proving highly cost-effective compared to traditional outpatient treatment. Recent economic analyses show that integrating structured physical activity like boxing leads to 34–47% reductions in total healthcare costs, as well as a 41% decrease in relapse-related emergency department visits statewide. These savings come from fewer hospitalizations, reduced relapse incidents, and improved employment outcomes—key business considerations for professionals seeking sustainable recovery. In metro regions such as Nashville and Knoxville, movement-based interventions may involve higher up-front program costs but deliver superior long-term value by accelerating engagement and retention. For many, this approach represents a strategic investment in both health and productivity.10
Boxing therapy Tennessee, when delivered without proper screening or clinical oversight, can potentially trigger re-traumatization—especially in men with complex PTSD. Research highlights that combat-based interventions activate the body’s threat-detection systems; this is therapeutic when managed within a controlled, supportive environment but may overwhelm individuals if exposure is not carefully titrated. State guidelines require licensed clinicians to assess trauma history, monitor for acute stress reactions, and implement individualized safety plans before participation. Evidence shows that, with these protocols in place, boxing therapy is not only safe but also highly effective for trauma processing, minimizing the risk of emotional harm while maximizing positive outcomes.2,7
Coverage for boxing therapy Tennessee as part of addiction treatment is expanding, but varies by insurer and program region. Some of the state’s major health plans—including several operating in Nashville and Knoxville—have begun reimbursing movement-based interventions when delivered within licensed, evidence-based addiction treatment frameworks and supervised by qualified clinicians. Recent state health policy updates encourage insurance providers to recognize boxing therapy as a clinically-supported complement to standard care, especially in dual diagnosis programs. However, coverage specifics—such as prior authorization or plan exclusions—differ between providers. Professionals are encouraged to verify benefit details with their insurer and seek programs that meet Tennessee’s clinical standards for reimbursement eligibility.2,9
Most participants in boxing therapy Tennessee begin to notice measurable outcomes within four to six weeks of consistent engagement. Peer-reviewed studies report that this timeframe is sufficient to produce significant neurobiological changes—such as increased vagal tone and improved brain-derived neurotrophic factor (BDNF) levels—that translate into better emotional regulation, reduced cravings, and enhanced sleep quality. For many men attending programs in Nashville, Knoxville, or rural areas, early improvements include sharper focus, more stable moods, and greater resilience to stressors. While individual progress varies based on trauma history and program intensity, the majority achieve noticeable benefits by the end of their first month of structured sessions.1,6
Screening protocols for boxing therapy Tennessee follow strict state and clinical guidelines to ensure participant safety. Before starting, licensed clinicians conduct comprehensive intake assessments that include mental health histories, substance use patterns, trauma screening, and physical health checks 2. Special attention is given to identifying acute psychiatric symptoms, suicidality, or cardiovascular risks that might contraindicate participation. For men with complex PTSD or recent trauma exposure, individualized safety planning is required; this may include trauma-informed interviews and ongoing risk monitoring during sessions. Only those meeting clinical criteria and able to participate safely are cleared, with peer facilitators supporting under direct supervision by credentialed professionals.9
Yes, Nashville and Knoxville programs offering boxing therapy Tennessee routinely accept out-of-state participants, provided clinical and regulatory criteria are met. State regulations require all participants—regardless of residency—to complete comprehensive intake assessments and demonstrate appropriateness for movement-based interventions under licensed clinical supervision. Demand from out-of-state professionals and veterans has grown as Tennessee’s male-specific, movement-oriented models gain recognition for their effectiveness and rigorous oversight. Insurance coverage for non-residents may vary, especially for those traveling from outside the Southeast, so verifying benefits and program eligibility is essential. Admission processes remain streamlined to accommodate out-of-state applicants, reflecting Tennessee’s commitment to accessibility and regional leadership in active recovery.2,9


April 13, 2026

April 15, 2026

April 15, 2026